Ansa cervicalis stimulation effects on upper airway patency: a structure-based analysis
- PMID: 39401858
- PMCID: PMC11740831
- DOI: 10.1183/13993003.00901-2024
Ansa cervicalis stimulation effects on upper airway patency: a structure-based analysis
Abstract
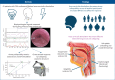
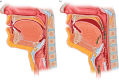
Rationale: Ansa cervicalis stimulation (ACS) of the infrahyoid muscles has been proposed as a neurostimulation therapy for obstructive sleep apnoea (OSA). ACS stabilises the pharynx by pulling it caudally, but its specific effects on flow limitation caused by palatal, oropharyngeal lateral wall, tongue base, or epiglottis collapse remains unclear.
Objectives: To quantify the effect of ACS on collapsibility of different pharyngeal flow-limiting structures.
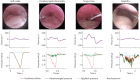
Methods: Participants with OSA underwent bilateral ACS during drug-induced sleep endoscopy. Maximum inspiratory airflow was assessed over a range of positive airway pressures while ACS was applied. The flow-limiting structure for each breath was classified based on manometric and endoscopic findings and a linear mixed-effects model characterised their response to ACS. The influence of patient characteristics was explored with univariate models.
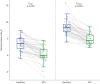
Measurements and main results: 41 participants yielded 1761 breaths for analysis. On average, bilateral ACS decreased the observed pharyngeal critical closing (P CRIT) and opening (P OPEN) pressures by -3.0 (95% CI -3.6--2.3) and -3.7 (-4.4--3.0) cmH2O, respectively (p<0.001). During tongue base obstruction, modelled ACS effects for P CRIT and P OPEN were -2.0 (-2.7--1.4) and -3.1 (-3.8--2.4) cmH2O, respectively (p<0.001). Greater reductions were generally observed for other flow-limiting structures. A lower apnoea-hypopnea index was associated with a greater decrease in P OPEN (p<0.01). Other patient characteristics, including body mass index, did not influence P CRIT or P OPEN (p>0.05).
Conclusions: Bilateral ACS decreased collapsibility of all airway flow-limiting structures. ACS generally had greater effects on palatal, oropharyngeal lateral wall and epiglottic collapse than the tongue base.
Copyright ©The authors 2025.
Conflict of interest statement
Conflict of interest: A.R. Schwartz is a scientific advisor for Apnimed, HuMannity Foundation, Invicta Medical, Itamar/Zoll, LivaNova, Lunair, Nyxoah SA, Periodic Breathing LLC, Respicardia/Zoll and Sonosa. C.J. Lindsell reports grants from NIH and Department of Defense and research funds from the CDC, biomeme, Novartis, bioMerieux, AstraZeneca, AbbVie, Entegrion Inc. and Endpoint Health, outside the submitted work, patents for risk stratification in sepsis and septic shock issued to Cincinnati Children's Hospital Medical Center, service on data safety monitoring board or advisory boards unrelated to the current work, stock options in Bioscape Digital unrelated to the current work, and is editor in chief of the Journal of Clinical and Translational Science. D.T. Kent has received research support from Invicta Medical, Inspire Medical System, and Nyxoah SA, is a consultant to Invicta Medical and Nyxoah SA, is a scientific advisory board member with Nyxoah SA, and is an inventor on patent pending PCT/US2020/021359 and related work licensed by Nyxoah SA that is relevant to this work. The remaining authors have no potential conflicts of interest to disclose.
Figures

Comment in
-
On the role of ansa cervicalis stimulation in the era of personalised medicine.Eur Respir J. 2025 Jan 16;65(1):2402137. doi: 10.1183/13993003.02137-2024. Print 2025 Jan. Eur Respir J. 2025. PMID: 39819826 No abstract available.
Similar articles
-
Ansa cervicalis stimulation increases pharyngeal patency in patients with obstructive sleep apnea.J Appl Physiol (1985). 2021 Aug 1;131(2):487-495. doi: 10.1152/japplphysiol.00076.2021. Epub 2021 Jul 1. J Appl Physiol (1985). 2021. PMID: 34197226 Free PMC article.
-
Effect of Sleeping Position on Upper Airway Patency in Obstructive Sleep Apnea Is Determined by the Pharyngeal Structure Causing Collapse.Sleep. 2017 Mar 1;40(3):zsx005. doi: 10.1093/sleep/zsx005. Sleep. 2017. PMID: 28329099 Free PMC article.
-
Polysomnographic airflow shapes and site of collapse during drug-induced sleep endoscopy.Eur Respir J. 2024 Jun 6;63(6):2400261. doi: 10.1183/13993003.00261-2024. Print 2024 Jun. Eur Respir J. 2024. PMID: 38548291 Free PMC article.
-
LwPTL: a novel classification for upper airway collapse in sleep endoscopies.Braz J Otorhinolaryngol. 2019 May-Jun;85(3):379-387. doi: 10.1016/j.bjorl.2019.01.010. Epub 2019 Mar 8. Braz J Otorhinolaryngol. 2019. PMID: 30902587 Free PMC article. Review.
-
[Progress in electrical stimulation on upper airway dilating muscles for treatment of obstructive sleep apnea].Zhonghua Jie He He Hu Xi Za Zhi. 2013 Mar;36(3):210-2. Zhonghua Jie He He Hu Xi Za Zhi. 2013. PMID: 23856146 Review. Chinese. No abstract available.
Cited by
-
Role of Glossopharyngeal Nerve Stimulation in Stabilizing the Lateral Pharyngeal Wall and Ventilation in OSA: A Pilot Study.Chest. 2025 May;167(5):1493-1496. doi: 10.1016/j.chest.2025.02.009. Epub 2025 Feb 18. Chest. 2025. PMID: 39978725 Free PMC article. No abstract available.
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
