Effects of Switching FSH Preparations on Sperm Parameters and Pregnancy: A Prospective Controlled Study
- PMID: 39407726
- PMCID: PMC11477313
- DOI: 10.3390/jcm13195666
Effects of Switching FSH Preparations on Sperm Parameters and Pregnancy: A Prospective Controlled Study
Abstract
Objective: To study the effect of switching to a follicle-stimulating hormone (FSH) preparation other than that to which infertile male patients have not had an effective response. Patients and methods: Seventy-four normogonadotropinemic, non-obstructive, oligozoospermic patients who were poor responders to the administration of highly purified FSH (hpFSH) (Group 1 (n = 22) and Group 3 (n = 15)) or to recombinant human FSH (rhFSH) (Group 2 (n = 22) and Group 4 (n = 15)) were selected for this prospective study. After 3 months of washout from treatment with the first FSH preparation of choice, rhFSH was administered to patients in Groups 1 and 4 and hpFSH to those in Groups 2 and 3. Serum luteinizing hormone, FSH, total testosterone levels, conventional sperm parameters, testicular volume, and the number of pregnancies were evaluated at study entry and after the first and second treatment cycles. Results: Comparing treatment groups, the greatest improvement in sperm parameters was recorded in the groups of patients prescribed the switch in FSH preparation. Group 1 had the greatest benefit from therapy, with the highest pregnancy rate after the second treatment cycle. Indeed, eight couples achieved pregnancy (36.4%), compared to Groups 2 (n = 4; 18.2%), 3 (n = 1; 6.7%), and 4 (n = 2; 13.3%) (p = 0.04). Conclusions: The results of this study suggest that a therapeutic scheme involving the "switching" of the FSH preparation yields better results than a protocol using the same FSH preparation for six months. These findings, if confirmed by further studies, will help us better design a treatment strategy with FSH for infertile patients with oligozoospermia.
Keywords: FSH; hpFSH; pregnancy; rhFSH; sperm concentration; switch; therapeutic scheme; total sperm count.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
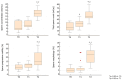
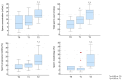
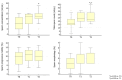
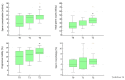
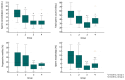
References
-
- [(accessed on 20 August 2023)]. Available online: https://www.who.int/news/item/04-04-2023-1-in-6-people-globally-affected....
-
- Thonneau P., Marchand S., Tallec A., Ferial M.L., Ducot B., Lansac J., Lopes P., Tabaste J.M., Spira A. Incidence and main causes of infertility in a resident population (1,850,000) of three French regions (1988–1989) Hum. Reprod. 1991;6:811–816. doi: 10.1093/oxfordjournals.humrep.a137433. - DOI - PubMed
LinkOut - more resources
Full Text Sources

