Is It Time for a New Algorithm for the Pharmacotherapy of Steroid-Induced Diabetes?
- PMID: 39407860
- PMCID: PMC11605232
- DOI: 10.3390/jcm13195801
Is It Time for a New Algorithm for the Pharmacotherapy of Steroid-Induced Diabetes?
Abstract
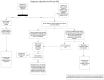
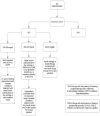
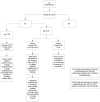
Glucocorticoids (GS) are widely used in multiple medical indications due to their anti-inflammatory, immunosuppressive, and antiproliferative effects. Despite their effectiveness in treating respiratory, skin, joint, renal, and neoplastic diseases, they dysregulate glucose metabolism, leading to steroid-induced diabetes (SID) or a significant increase of glycemia in people with previously diagnosed diabetes. The risk of adverse event development depends on the prior therapy, the duration of the treatment, the form of the drug, and individual factors, i.e., BMI, genetics, and age. Unfortunately, SID and steroid-induced hyperglycemia (SIH) are often overlooked, because the fasting blood glucose level, which is the most commonly used diagnostic test, is insufficient for excluding both conditions. The appropriate control of post-steroid hyperglycemia remains a major challenge in everyday clinical practice. Recently, the most frequently used antidiabetic strategies have been insulin therapy with isophane insulin or multiple injections in the basal-bolus regimen. Alternatively, in patients with lower glycemia, sulphonylureas or glinides were used. Taking into account the pathogenesis of post-steroid-induced hyperglycemia, the initiation of therapy with glucagon-like peptide 1 (GLP-1) analogs and dipeptidyl peptidase 4 (DPP-4) inhibitors should be considered. In this article, we present a universal practical diagnostic algorithm of SID/SIH in patients requiring steroids, in both acute and chronic conditions, and we present a new pharmacotherapy algorithm taking into account the use of all currently available antidiabetic drugs.
Keywords: diabetes; glucagon-like peptide 1 agonists; glucocorticoids; pharmacotherapy algorithm; steroid-induced diabetes.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


References
-
- Nowak K.M., Rdzanek-Pikus M., Romanowska-Próchnicka K., Nowakowska-Płaza A., Papierska L. High prevalence of steroid-induced glucose intolerance with normal fasting glycaemia during low-dose glucocorticoid therapy: An oral glucose tolerance test screening study. Rheumatology. 2021;60:2842–2851. doi: 10.1093/rheumatology/keaa724. - DOI - PubMed
-
- Boris D., Vanita R.A., George B., Gretchen B., Florence M.B., RaShaye F., Jennifer G., Elbert H., Diana I., Scott K. Diabetes Care in the Hospital: Standards of Medical Care in Diabetes-2022. Diabetes Care. 2022;45((Suppl. S1)):S244–S253.
-
- Pisarczyk-Wiza Dorota Z.-Z.D. Glucocortycosteroids and disturbances of glucose metabolism. Clin. Diabetol. 2015;4:110–116.
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

