A Comparative Study of Hospitalization Mortality Rates between General and Emergency Hospitalized Patients Using Survival Analysis
- PMID: 39408162
- PMCID: PMC11476090
- DOI: 10.3390/healthcare12191982
A Comparative Study of Hospitalization Mortality Rates between General and Emergency Hospitalized Patients Using Survival Analysis
Abstract
Background/objectives: In Korea's emergency medical system, when an emergency patient arises, patients receive on-site treatment and care during transport at the pre-hospital stage, followed by inpatient treatment upon hospitalization. From the perspective of emergency patient management, it is critical to identify the high death rate of patients with certain conditions in the emergency room. Therefore, it is necessary to compare and analyze the determinants of the death rate of patients admitted via the emergency room and generally hospitalized patients. In fact, previous studies investigating determinants of survival periods or length of stay (LOS) primarily used multiple or logistic regression analyses as their main research methodology. Although medical data often exhibit censored characteristics, which are crucial for analyzing survival periods, the aforementioned methods of analysis fail to accommodate these characteristics, presenting a significant limitation.
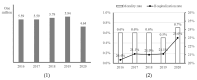
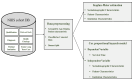
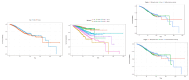
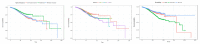
Methods: Therefore, in this study, survival analyses were performed to investigate factors affecting the dying risk of general inpatients as well as patients admitted through the emergency room. For this purpose, this study collected and analyzed the sample cohort DB for a total of four years from 2016 to 2019 provided by the Korean National Health Insurance Services (NHIS). After data preprocessing, the survival probability was estimated according to sociodemographic, patient, health checkup records, and institutional features through the Kaplan-Meier survival estimation. Then, the Cox proportional hazards models were additionally utilized for further econometric validation.
Results: As a result of the analysis, in terms of the 'city' feature among the sociodemographic characteristics, the small and medium-sized cities exert the most influence on the death rate of general inpatients, whereas the metropolitan cities exert the most influence on the death rate of inpatients admitted through the emergency room. In terms of institution characteristics, it was found that there is a difference in determinants affecting the death rate of the two groups of study, such as the number of doctors per 100 hospital beds, the number of nurses per 100 hospital beds, the number of hospital beds, the number of surgical beds, and the number of emergency beds.
Conclusions: Based on the study results, it is expected that an efficient plan for distributing limited medical resources can be established based on inpatients' LOS.
Keywords: Kaplan–Meier survival analysis; cox proportional hazards model; death rate; medical data; national health insurance services cohort DB; survival analysis; survival period.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

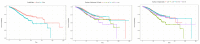





References
-
- Yoon K.J. Infectious diseases and public healthcare through the response to COVID-19. Health Welf. Issue Focus. 2020;377:1–11.
-
- Oh Y.H. Problems and policy directions of the emergency medical system in Korea. Health Welf. Issue Focus. 2011;105:1–8.
-
- Jeon B., Kim K., Jin Y. Ontology Design to Improve User Fitness of Emergency Medical Statistics Quality(EMSQ) J. Korea Acad.-Ind. Coop. Soc. 2024;25:208–215.
-
- Hwang H.E., Kahng H., Lee E.S., Kim J.Y., Yoon Y.H., Kim S.B. Early Prediction of Patient Disposition for Emergency Department Visits Using Machine Learning. J. Korean Inst. Ind. Eng. 2021;47:263–271.
-
- Jung G.H., Kweon J. A study on space use analysis at emergency room in local emergency medical center. J. Digit. Des. 2017;17:81–92.
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

