Genetic Analysis of Biopsy Tissues from Colorectal Tumors in Patients with Ulcerative Colitis
- PMID: 39409892
- PMCID: PMC11475702
- DOI: 10.3390/cancers16193271
Genetic Analysis of Biopsy Tissues from Colorectal Tumors in Patients with Ulcerative Colitis
Abstract
Background/objectives: Colorectal neoplasia developing from ulcerative colitis mucosa (CRNUC) can be divided into ulcerative colitis-associated neoplasia (UCAN) and non-UCAN; however, it is often difficult to distinguish UCAN from non-UCAN during a biopsy diagnosis. We investigated whether a genomic analysis could improve the diagnostic accuracy of UCAN using biopsy specimens.
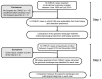
Methods: In step 1, 14 CRNUCs were used to examine whether the genomic landscape of biopsy and resection specimens matched. In step 2, we investigated the relationship between the genomic landscapes and the pathological diagnosis of 26 CRNUCs. The cancer genome was analyzed by deep sequencing using a custom panel of 27 genes found to be mutated in our previous CRNUC analysis.
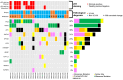
Results: In step 1, of the 27 candidate genes, 14 were mutated. The concordance rate of the pathogenic mutations in these 14 genes between the biopsy and resection specimens was 29% (4/14), while that of the pathogenic mutations in TP53 and KRAS was 79% (11/14). In step 2, the pathological diagnosis of biopsy specimens using only hematoxylin and eosin (HE) staining had a sensitivity of 33% and an accuracy of 38% for UCAN diagnosis. On the other hand, the combination of the HE pathology and p53 immunohistochemical staining had a sensitivity of 73% and an accuracy of 85% for UCAN diagnosis, while the combination of HE staining and a TP53 mutation had a sensitivity of 87% and an accuracy of 88% for UCAN diagnosis.
Conclusions: An evaluation of TP53 mutations in biopsy specimens may be useful for diagnosing UCAN. However, further studies with larger sample sizes are required before this can be applied in clinical practice.
Keywords: TP53 mutation; biopsy; sporadic neoplasia; ulcerative colitis; ulcerative colitis-associated neoplasia.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Ng S.C., Shi H.Y., Hamidi N., Underwood F.E., Tang W., Benchimol E.I., Panaccione R., Ghosh S., Wu J.C.Y., Chan F.K.L., et al. Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: A systematic review of population-based studies. Lancet. 2017;390:2769–2778. doi: 10.1016/S0140-6736(17)32448-0. - DOI - PubMed
-
- Eriksson C., Cao Y., Rundquist S., Zhulina Y., Henriksson I., Montgomery S., Halfvarson J. Changes in medical management and colectomy rates: A population-based cohort study on the epidemiology and natural history of ulcerative colitis in Örebro, Sweden, 1963–2010. Aliment. Pharmacol. Ther. 2017;46:748–757. doi: 10.1111/apt.14268. - DOI - PubMed
-
- Noguchi T., Ishihara S., Uchino M., Ikeuchi H., Okabayashi K., Futami K., Tanaka S., Ohge H., Nagahara H., Watanabe K., et al. Clinical features and oncological outcomes of intestinal cancers associated with ulcerative colitis and Crohn’s disease. J. Gastroenterol. 2023;58:14–24. doi: 10.1007/s00535-022-01927-y. - DOI - PubMed
-
- Uchino M., Ikeuchi H., Hata K., Okada S., Ishihara S., Morimoto K., Sahara R., Watanabe K., Fukushima K., Takahashi K., et al. Changes in the rate of and trends in colectomy for ulcerative colitis during the era of biologics and calcineurin inhibitors based on a Japanese nationwide cohort study. Surg. Today. 2019;49:1066–1073. doi: 10.1007/s00595-019-01845-2. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

