Development and Evaluation of Pediatric Acute Care Hospital Referral Regions in Eight States
- PMID: 39423908
- PMCID: PMC12007411
- DOI: 10.1016/j.jpeds.2024.114371
Development and Evaluation of Pediatric Acute Care Hospital Referral Regions in Eight States
Abstract
Objective: To develop a set of pediatric acute care hospital referral regions for use in studying pediatric acute care delivery and test their utility relative to other regional systems.
Study design: We used state-level administrative databases capturing all pediatric acute care in 8 states to construct novel referral regions. We first constructed pediatric hospital service areas (PHSAs) based on 5 837 464 pediatric emergency department encounters. We then aggregated these PHSAs to pediatric hospital referral regions (PHRRs) based on 344 440 pediatric hospitalizations. Finally, we used 3 measures of spatial accuracy (localization index, market share index, and net patient flow) to compare this novel region system with the Dartmouth Atlas, designed originally to study adult specialty care, and the Pittsburgh Atlas, designed originally to study adult acute care.
Results: The development procedure resulted in 717 novel PHSAs, which were then aggregated to 55 PHRRs across the included states. Relative to hospital referral regions in the Dartmouth and Pittsburgh Atlases, PHRRs were fewer in number and larger in area and population. PHRRs more accurately captured patterns of pediatric hospitalizations, (eg, mean localization index: 69.1 out of 100, compared with a mean of 58.1 for the Dartmouth Atlas and 62.4 for the Pittsburgh Atlas).
Conclusions: The use of regional definitions designed specifically to study pediatric acute care better captures contemporary pediatric acute care delivery than the use of existing regional definitions. Future work should extend these definitions to all US states to enable national analyses of pediatric acute care delivery.
Keywords: acute care; emergency medicine; geography; hospital medicine; pediatrics; regionalization.
Copyright © 2024 The Author(s). Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Declaration of Competing Interest Prof. Kurland has received compensation for textbook authorship from Esri, Inc, the maker of ArcGIS software used in this project. Dr Joseph was supported by a grant from the National Institutes of Health (5T32HL007820). The NIH had no role in the study design, data analysis, manuscript preparation, or decision to submit the manuscript for publication.
Figures


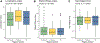
Similar articles
-
Assessment of Acute Hospital Use and Transfers for Management of Pediatric Seizures.JAMA Netw Open. 2020 Apr 1;3(4):e203148. doi: 10.1001/jamanetworkopen.2020.3148. JAMA Netw Open. 2020. PMID: 32315068 Free PMC article.
-
The Utility of a Novel Definition of Health Care Regions in the United States in the Era of COVID-19: A Validation of the Pittsburgh Atlas Using Pneumonia Admissions.Ann Emerg Med. 2022 Jun;79(6):518-526. doi: 10.1016/j.annemergmed.2021.11.017. Epub 2021 Nov 25. Ann Emerg Med. 2022. PMID: 34952728 Free PMC article.
-
Referral Regions for Time-Sensitive Acute Care Conditions in the United States.Ann Emerg Med. 2018 Aug;72(2):147-155. doi: 10.1016/j.annemergmed.2018.02.018. Epub 2018 Mar 29. Ann Emerg Med. 2018. PMID: 29606286 Free PMC article.
-
Use of a National Database to Assess Pediatric Emergency Care Across United States Emergency Departments.Acad Emerg Med. 2018 Dec;25(12):1355-1364. doi: 10.1111/acem.13489. Epub 2018 Jul 4. Acad Emerg Med. 2018. PMID: 29858524
-
Sociodemographic Factors Associated With Adherence to Referrals From the Pediatric Emergency Department.J Emerg Med. 2020 Apr;58(4):594-602. doi: 10.1016/j.jemermed.2019.11.023. Epub 2020 Jan 23. J Emerg Med. 2020. PMID: 31982196 Review.
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

