Clinical Outcomes of a Novel Multidisciplinary Care Program in Advanced Kidney Disease (PEAK)
- PMID: 39430180
- PMCID: PMC11489444
- DOI: 10.1016/j.ekir.2024.07.018
Clinical Outcomes of a Novel Multidisciplinary Care Program in Advanced Kidney Disease (PEAK)
Abstract
Introduction: Multidisciplinary care (MDC) for late-stage chronic kidney disease (CKD) has been associated with improved patient outcomes compared with traditional nephrology care; however, the optimal MDC model is unknown. In 2015, we implemented a novel MDC model for patients with late-stage CKD informed by the Chronic Care Model conceptual framework, including an expanded MDC team, care plan meetings, clinical risk prediction, and a patient dashboard.
Methods: We conducted a single-center, retrospective cohort study of adults with late-stage CKD (estimated glomerular filtration rate [eGFR] < 30 ml/min per 1.73 m2) enrolled from May 2015 to February 2020 in the Program for Education in Advanced Kidney Disease (PEAK). Our primary composite outcome was an optimal transition to end-stage kidney disease (ESKD) defined as starting in-center hemodialysis (ICHD) as an outpatient with an arteriovenous fistula (AVF) or graft (AVG), or receiving home dialysis, or a preemptive kidney transplant. Secondary outcomes included home dialysis initiation, preemptive transplantation, vascular access at dialysis initiation, and location of ICHD initiation. We used logistic regression to examine trends in outcomes. Results were stratified by race, ethnicity, and insurance payor, and compared with national and regional averages from the United States Renal Data System (USRDS) averaged from 2015 to 2019.
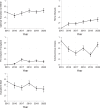
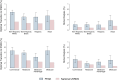
Results: Among 489 patients in the PEAK program, 37 (8%) died prior to ESKD and 151 (31%) never progressed to ESKD. Of the 301 patients (62%) who progressed to ESKD, 175 (58%) achieved an optimal transition to ESKD, including 54 (18%) on peritoneal dialysis, 16 (5%) on home hemodialysis, and 36 (12%) to preemptive transplant. Of the 195 patients (65%) starting ICHD, 51% started with an AVF or AVG and 52% started as an outpatient. The likelihood of starting home dialysis increased by 1.34 times per year from 2015 to 2020 (95% confidence interval [CI]: 1.05-1.71, P = 0.018) in multivariable adjusted results. Optimal transitions to ESKD and home dialysis rates were higher than the national USRDS data (58% vs. 30%; 23% vs. 11%) across patient race, ethnicity, and payor.
Conclusion: Patients enrolled in a novel comprehensive MDC model coupled with risk prediction and health information technology were nearly twice as likely to achieve an optimal transition to ESKD and start dialysis at home, compared with national averages.
Keywords: chronic care model; health information technology; home dialysis; late-stage chronic kidney disease; multidisciplinary care; optimal starts.
© 2024 International Society of Nephrology. Published by Elsevier Inc.
Figures


References
-
- United States Renal Data System . 2023 USRDS Annual Data Report: Epidemiology of kidney disease in the United States. National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases; 2023.
-
- Crooks P.W., Thomas C.O., Compton-Phillips A., et al. Clinical outcomes and healthcare use associated with optimal ESRD starts. Am J Manag Care. 2018;24:e305–e311. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

