Anastomotic leak after manual circular stapled left-sided bowel surgery: analysis of technology-, disease-, and patient-related factors
- PMID: 39441693
- PMCID: PMC11498054
- DOI: 10.1093/bjsopen/zrae089
Anastomotic leak after manual circular stapled left-sided bowel surgery: analysis of technology-, disease-, and patient-related factors
Abstract
Background: Anastomotic leak rates after colorectal surgery remain high. In most left-sided colon and rectal resection surgeries, a circular stapler is utilized to create the primary bowel anastomosis. However, it remains unclear whether a relationship between circular stapler technology and anastomotic leak in left-sided colorectal surgery exists.
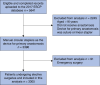
Methods: A post-hoc analysis was conducted using a prospectively collected data set of patients from the 2017 European Society of Coloproctology snapshot audit who underwent elective left-sided resection (left hemicolectomy, sigmoid colectomy, or rectal resection) with a manual circular stapled anastomosis. Rates of anastomotic leak and unplanned intensive care unit stay in association with manual circular stapling were assessed. Patient-, disease-, geographical-, and surgeon-related factors as well as stapler brand were explored using multivariable regression models to identify predictors of adverse outcomes.
Results: Across 3305 procedures, 8.0% of patients had an anastomotic leak and 2.1% had an unplanned intensive care unit stay. Independent predictors of anastomotic leak were male sex, minimal-access surgery converted to open surgery, and anastomosis height C11 (lower third rectum) (all P < 0.050). Independent predictors of unplanned intensive care unit stay were minimal-access surgery converted to open surgery and American Society of Anesthesiologists grade IV (all P < 0.050). Stapler device brand was not a predictor of anastomotic leak or unplanned intensive care unit stay in multivariable regression analysis. There were no differences in rates of anastomotic leak and unplanned intensive care unit stay according to stapler head diameter, geographical region, or surgeon experience.
Conclusion: In patients undergoing left-sided bowel anastomosis, choice of manual circular stapler, in terms of manufacturer or head diameter, is not associated with rates of anastomotic leak and unplanned intensive care unit stay.
© The Author(s) 2024. Published by Oxford University Press on behalf of BJS Foundation Ltd.
Figures
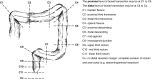


References
-
- European Society of Coloproctology Collaborating Group . 2017 ESCP Snapshot Audit, Study Protocol: Left Colon, Sigmoid and Rectal Resections (Version 2.5). 2017. https://www.escp.eu.com/images/research/documents/2017-ESCP-snapshot-aud... (accessed 31 August 2024)
-
- Ashraf SQ, Burns EM, Jani A, Altman S, Young JD, Cunningham C et al. The economic impact of anastomotic leakage after anterior resections in English NHS hospitals: are we adequately remunerating them? Colorectal Dis 2013;15:e190–e198 - PubMed
-
- Frye J, Bokey EL, Chapuis PH, Sinclair G, Dent OF. Anastomotic leakage after resection of colorectal cancer generates prodigious use of hospital resources. Colorectal Dis 2009;11:917–920 - PubMed

