Focal Unspecific Bone Uptake on [18F]PSMA-1007 PET: Evaluation Analog PROMISE Criteria and Validation via PET/CT Follow-Up
- PMID: 39451650
- PMCID: PMC11506528
- DOI: 10.3390/diagnostics14202327
Focal Unspecific Bone Uptake on [18F]PSMA-1007 PET: Evaluation Analog PROMISE Criteria and Validation via PET/CT Follow-Up
Abstract
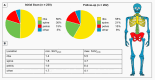
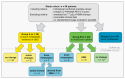
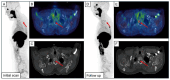
Background: Focal unspecific bone uptake (UBU) is common in [18F]PSMA-1007 PET/CT, yet its clinical significance remains unclear, causing uncertainty in treatment decisions. Material and Methods: We retrospectively analyzed 99 prostate cancer patients (age 69 ± 7) who underwent [18F]PSMA-1007 PET/CT scans (3 MBq/kg; uptake time 70 ± 14 min) for staging and follow-up (after 13.0 ± 7.2 months). Semiquantitative assessment using the miPSMA score, analogous to the PROMISE criteria, evaluated the prevalence of UBU and bone metastases. Results: In the initial PET/CT scan, 56 patients had 230 lesions classified as UBU. A total of 19 patients were found to have bone metastases and UBU, while 24 patients had no focal bone uptake. UBU distribution was as follows: ribs (50%), spine (30%), pelvis (15%), and other sites (5%). There were no significant differences in age, Gleason score, injected tracer dose, uptake time, SUVpeak of UBU, or SUVmean in the spleen and parotid gland between patients with and without UBU. Follow-up showed stable miPSMA-score and CT appearance in 44/56 patients with UBU (79%), minor changes in 5/56 patients (8%), and new bone metastases in 7/56 patients (12%). Patient-specific analysis indicated at least one bone metastasis initially classified as UBU in 3/56 patients (5%) and new bone metastases in 4/56 patients (7%). In total, 4 of the 24 patients (17%) without initial focal uptake developed osseous metastases at follow-up. Conclusions: No significant differences were found between patients with or without UBU. Only a small portion of UBU (2%) evolved into metastases, a lower rate than the development of new osseous metastases, which appears to be independent of UBU.
Keywords: PET/CT; [18F]PSMA-1007; bone lesion; bone metastases; prostate cancer; unspecific bone uptake.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

References
-
- Hofman M.S., Lawrentschuk N., Francis R.J., Tang C., Vela I., Thomas P., Rutherford N., Martin J.M., Frydenberg M., Shakher R., et al. Prostate-specific membrane antigen PET-CT in patients with high-risk prostate cancer before curative-intent surgery or radiotherapy (proPSMA): A prospective, randomised, multicentre study. Lancet. 2020;395:1208–1216. doi: 10.1016/S0140-6736(20)30314-7. - DOI - PubMed
-
- Perera M., Papa N., Christidis D., Wetherell D., Hofman M.S., Murphy D.G., Bolton D., Lawrentschuk N. Sensitivity, Specificity, and Predictors of Positive (68)Ga-Prostate-specific Membrane Antigen Positron Emission Tomography in Advanced Prostate Cancer: A Systematic Review and Meta-analysis. Eur. Urol. 2016;70:926–937. doi: 10.1016/j.eururo.2016.06.021. - DOI - PubMed
-
- Fendler W.P., Calais J., Eiber M., Flavell R.R., Mishoe A., Feng F.Y., Nguyen H.G., Reiter R.E., Rettig M.B., Okamoto S., et al. Assessment of 68Ga-PSMA-11 PET Accuracy in Localizing Recurrent Prostate Cancer: A Prospective Single-Arm Clinical Trial. JAMA Oncol. 2019;5:856–863. doi: 10.1001/jamaoncol.2019.0096. - DOI - PMC - PubMed
-
- Janssen J.C., Meissner S., Woythal N., Prasad V., Brenner W., Diederichs G., Hamm B., Makowski M.R. Comparison of hybrid (68)Ga-PSMA-PET/CT and (99m)Tc-DPD-SPECT/CT for the detection of bone metastases in prostate cancer patients: Additional value of morphologic information from low dose CT. Eur. Radiol. 2018;28:610–619. doi: 10.1007/s00330-017-4994-6. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

