Size-Sorted Superheated Nanodroplets for Dosimetry and Range Verification of Carbon-Ion Radiotherapy
- PMID: 39452979
- PMCID: PMC11509999
- DOI: 10.3390/nano14201643
Size-Sorted Superheated Nanodroplets for Dosimetry and Range Verification of Carbon-Ion Radiotherapy
Abstract
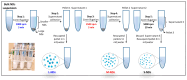
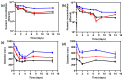
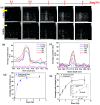
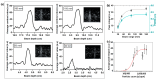
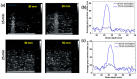
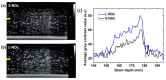
Nanodroplets have demonstrated potential for the range detection of hadron radiotherapies. Our formulation uses superheated perfluorobutane (C4F10) stabilized by a poly(vinyl-alcohol) shell. High-LET (linear energy transfer) particles vaporize the nanodroplets into echogenic microbubbles. Tailored ultrasound imaging translates the generated echo-contrast into a dose distribution map, enabling beam range retrieval. This work evaluates the response of size-sorted nanodroplets to carbon-ion radiation. We studied how thesize of nanodroplets affects their sensitivity at various beam-doses and energies, as a function of concentration and shell cross-linking. First, we show the physicochemical characterization of size-isolated nanodroplets by differential centrifugation. Then, we report on the irradiations of the nanodroplet samples in tissue-mimicking phantoms. We compared the response of large (≈900 nm) and small (≈400 nm) nanodroplets to different carbon-ions energies and evaluated their dose linearity and concentration detection thresholds by ultrasound imaging. Additionally, we verified the beam range detection accuracy for the nanodroplets samples. All nanodroplets exhibited sensitivity to carbon-ions with high range verification precision. However, smaller nanodroplets required a higher concentration sensitivity threshold. The vaporization yield depends on the carbon-ions energy and dose, which are both related to particle count/spot. These findings confirm the potential of nanodroplets for range detection, with performance depending on nanodroplets' properties and beam parameters.
Keywords: carbon-ions radiotherapy; dosimetry; nanodroplets; range verification; ultrasound imaging.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



References
-
- Kirkby K.J., Kirkby N.F., Burnet N.G., Owen H., Mackay R.I., Crellin A., Green S. Heavy charged particle beam therapy and related new radiotherapy technologies: The clinical potential, physics and technical developments required to deliver benefit for patients with cancer. Br. J. Radiol. 2020;93:20200247. doi: 10.1259/bjr.20200247. - DOI - PMC - PubMed
-
- PTCOG—Facilities in Operation. [(accessed on 10 July 2024)]. Available online: https://www.ptcog.site/index.php/facilities-in-operation-public.
-
- Kohno R., Koto M., Ikawa H., Lee S.H., Sato K., Hashimoto M., Inaniwa T., Shirai T. High–Linear Energy Transfer Irradiation in Clinical Carbon-Ion Beam With the Linear Energy Transfer Painting Technique for Patients With Head and Neck Cancer. Adv. Radiat. Oncol. 2024;9:101317. doi: 10.1016/j.adro.2023.101317. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

