Respiratory Syncytial Virus and US Pediatric Intensive Care Utilization
- PMID: 39453655
- PMCID: PMC11581606
- DOI: 10.1001/jamanetworkopen.2024.40997
Respiratory Syncytial Virus and US Pediatric Intensive Care Utilization
Erratum in
-
Error in Introduction.JAMA Netw Open. 2025 Mar 3;8(3):e254977. doi: 10.1001/jamanetworkopen.2025.4977. JAMA Netw Open. 2025. PMID: 40029666 Free PMC article. No abstract available.
Abstract
Importance: Bronchiolitis is the most common diagnosis necessitating respiratory support and pediatric intensive care, and respiratory syncytial virus (RSV) is the most common cause of bronchiolitis. In 2023, the monoclonal antibody nirsevimab and the maternal RSVpreF vaccine were implemented to prevent RSV in infants.
Objective: To determine the potential association of novel RSV prevention strategies with pediatric intensive care unit (ICU) utilization.
Design, setting, and participants: This retrospective cross-sectional study examined US pediatric ICU encounters with and without RSV from January 1, 2017, to June 1, 2023. Data were from Oracle Cerner RealWorld Data, a national electronic health record database. All children (aged >1 day and <18 years) admitted to an ICU during the study period were included in the analysis. Statistical analysis was performed from February to May 2024.
Main outcomes and measures: The primary outcomes were ICU encounters with RSV and ICU encounters with RSV eligible for RSV prevention.
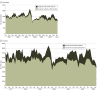
Results: There were 119 782 ICU encounters from 53 hospitals; 65 757 encounters (54.9%) were male; median (IQR) age was 4.5 (1.1-12.5) years, median (IQR) ICU length of stay was 1.8 (1.0-3.9) days; 13 702 ICU encounters (11.4%) had RSV, of which 38.6% (5217) were eligible for prevention (4.4% of total ICU encounters). Encounters with RSV accounted for 21.1% (109 334) of ICU days, of which 43.8% (47 888) were eligible for prevention (9.2% of total ICU days). Encounters with RSV were associated with a greater use of positive pressure ventilation (4074 [29.7%] vs 18 821 [17.7%]; P < .001) and vasoactive medications (3057 [22.3%] vs 18 570 [17.5%]; P < .001) compared with those without RSV.
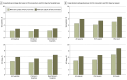
Conclusions and relevance: The findings of this retrospective cross-sectional study of RSV and US pediatric intensive care utilization suggest that if 65% to 85% of eligible children received RSV prevention, an estimated 2.1% to 2.8% reduction in pediatric ICU encounters and an estimated 4.5% to 5.9% reduction in pediatric ICU days could be achieved.
Conflict of interest statement
Figures
References
-
- Li Y, Wang X, Blau DM, et al. ; Respiratory Virus Global Epidemiology Network; RESCEU investigators . Global, regional, and national disease burden estimates of acute lower respiratory infections due to respiratory syncytial virus in children younger than 5 years in 2019: a systematic analysis. Lancet. 2022;399(10340):2047-2064. doi: 10.1016/S0140-6736(22)00478-0 - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

