Neutrophil Extracellular Traps in Pediatric Inflammatory Bowel Disease: A Potential Role in Ulcerative Colitis
- PMID: 39456908
- PMCID: PMC11507660
- DOI: 10.3390/ijms252011126
Neutrophil Extracellular Traps in Pediatric Inflammatory Bowel Disease: A Potential Role in Ulcerative Colitis
Abstract
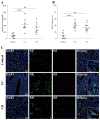
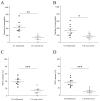
Inflammatory bowel disease (IBD), encompassing Crohn's disease (CD) and ulcerative colitis (UC), is a chronic inflammatory condition of the gut affecting both adults and children. Neutrophil extracellular traps (NETs) are structures released by activated neutrophils, potentially contributing to tissue damage in various diseases. This study aimed to explore the presence and role of NETs in pediatric IBD. We compared intestinal biopsies and peripheral blood from 20 pediatric IBD patients (UC and CD) to controls. Biopsy staining and techniques for neutrophil activation were used to assess neutrophil infiltration and NET formation. We also measured the enzymatic activity of key NET proteins and evaluated NET formation in UC patients in remission. Both UC and CD biopsies showed significantly higher levels of neutrophils and NETs compared to controls (p < 0.01), with UC exhibiting the strongest association. Peripheral blood neutrophils from UC patients at diagnosis displayed increased NET formation compared to controls and CD patients. Interestingly, NET formation normalized in UC patients following remission-inducing treatment. This pilot study suggests a potential role for NETs in pediatric IBD, particularly UC. These findings warrant further investigation into the mechanisms of NET involvement and the potential for targeting NET formation as a therapeutic strategy.
Keywords: Crohn’s disease; inflammatory bowel disease; neutrophil; neutrophil extracellular traps (NETs); prognostic factor; ulcerative colitis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



Similar articles
-
Neutrophil Extracellular Traps Sustain Inflammatory Signals in Ulcerative Colitis.J Crohns Colitis. 2019 May 27;13(6):772-784. doi: 10.1093/ecco-jcc/jjy215. J Crohns Colitis. 2019. PMID: 30715224
-
Translocator protein facilitates neutrophil-mediated mucosal inflammation in inflammatory bowel diseases.World J Gastroenterol. 2025 Jul 21;31(27):109239. doi: 10.3748/wjg.v31.i27.109239. World J Gastroenterol. 2025. PMID: 40741102 Free PMC article.
-
Neutrophil extracellular traps in pediatric inflammatory bowel disease.Pathol Int. 2018 Sep;68(9):517-523. doi: 10.1111/pin.12715. Epub 2018 Aug 22. Pathol Int. 2018. PMID: 30133056
-
Neutrophils and NETs in Pathophysiology and Treatment of Inflammatory Bowel Disease.Int J Mol Sci. 2025 Jul 23;26(15):7098. doi: 10.3390/ijms26157098. Int J Mol Sci. 2025. PMID: 40806230 Free PMC article. Review.
-
Neutrophil Extracellular Traps in Inflammatory Bowel Disease: Pathogenic Mechanisms and Clinical Translation.Cell Mol Gastroenterol Hepatol. 2021;12(1):321-333. doi: 10.1016/j.jcmgh.2021.03.002. Epub 2021 Mar 6. Cell Mol Gastroenterol Hepatol. 2021. PMID: 33689803 Free PMC article. Review.
Cited by
-
Neutrophil Extracellular Traps (NETs) in Immunity and Diseases: Second Edition.Int J Mol Sci. 2025 Jul 8;26(14):6563. doi: 10.3390/ijms26146563. Int J Mol Sci. 2025. PMID: 40724813 Free PMC article.
References
-
- Ng S.C., Shi H.Y., Hamidi N., Underwood F.E., Tang W., Benchimol E.I., Panaccione R., Ghosh S., Wu J.C., Chan F.K., et al. Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: A systematic review of population-based studies. Lancet. 2017;390:2769–2778. doi: 10.1016/S0140-6736(17)32448-0. - DOI - PubMed
MeSH terms
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

