Characteristics and Prognosis of "Acute Promyelocytic Leukemia-like" Nucleophosmin-1-Mutated Acute Myeloid Leukemia in a Retrospective Patient Cohort
- PMID: 39457595
- PMCID: PMC11505509
- DOI: 10.3390/biomedicines12102282
Characteristics and Prognosis of "Acute Promyelocytic Leukemia-like" Nucleophosmin-1-Mutated Acute Myeloid Leukemia in a Retrospective Patient Cohort
Abstract
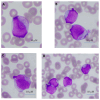
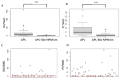
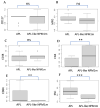
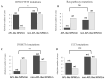
Background: AML with NPM1 mutation is the largest subcategory of AML, representing about 35% of AML cases. It is characterized by CD34 negativity, which suggests a relatively differentiated state of the bulk of leukemic blasts. Notably, a significant subset of NPM1-mutated AML cases also exhibit HLA-DR negativity, classifying them as "double-negative", and mimicking, therefore, the CD34- HLA-DR- immunophenotype of acute promyelocytic leukemia (APL). Objectives: This study focuses on the "acute promyelocytic leukemia-like" ("APL-like") subset of NPM1-mutated AML, which can be challenging to distinguish from APL at presentation, prior to confirming RARa translocations. We aim to investigate the hematologic and immunophenotypic parameters that may aid to its distinction from APL. Additionally, we explore differences in genetic profile and prognosis between "APL-like" and "non-APL-like" NPM1-mutated AML cases. Methods: We conducted a retrospective evaluation of 77 NPM1-mutated AML cases and 28 APL cases. Results: Morphological characteristics, hematologic parameters (such as DD/WBC and PT/WBC), and specific immunophenotypic markers (including SSC, CD64, and CD4) can assist in the early distinction of "APL-like" NPM1-mutated AML from APL. Regarding differences in genetic profiles and outcomes between "APL-like" and non-"APL-like" NPM1-mutated AML cases, we observed a significantly higher incidence of IDH1/2 /TET2 mutations, along with a significantly lower incidence of DNMT3A mutations in the "APL-like" subset compared to the non-"APL-like" subset. The frequency of Ras-pathway and FLT3 mutations did not differ between these last two groups, nor did their prognoses. Conclusions: Our findings contribute to a comprehensive characterization of NPM1-mutated AML, enhancing diagnostic accuracy and aiding in the detailed classification of the disease. This information may potentially guide targeted therapies or differentiation-based treatment strategies.
Keywords: AML with NPM1 mutation; DNMT3A mutations; FLT3 mutations; IDH1/2 mutations; Ras-pathway mutations; TET2 mutations; acute promyelocytic leukemia.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
Similar articles
-
A distinct immunophenotype identifies a subset of NPM1-mutated AML with TET2 or IDH1/2 mutations and improved outcome.Am J Hematol. 2018 Aug;93(4):504-510. doi: 10.1002/ajh.25018. Epub 2018 Jan 25. Am J Hematol. 2018. PMID: 29274134
-
Acute myeloid leukemia with mutated NPM1 mimics acute promyelocytic leukemia presentation.Int J Lab Hematol. 2021 Apr;43(2):218-226. doi: 10.1111/ijlh.13357. Epub 2020 Oct 25. Int J Lab Hematol. 2021. PMID: 33099879
-
Acute promyelocytic leukemia: Immunophenotype and differential diagnosis by flow cytometry.Cytometry B Clin Cytom. 2022 Jul;102(4):283-291. doi: 10.1002/cyto.b.22085. Epub 2022 Jun 18. Cytometry B Clin Cytom. 2022. PMID: 35716019
-
NPM1-mutated acute myeloid leukemia: New pathogenetic and therapeutic insights and open questions.Am J Hematol. 2023 Sep;98(9):1452-1464. doi: 10.1002/ajh.26989. Epub 2023 Jun 15. Am J Hematol. 2023. PMID: 37317978 Review.
-
Nucleophosmin gene mutations in acute myeloid leukemia.Arch Pathol Lab Med. 2006 Nov;130(11):1687-92. doi: 10.5858/2006-130-1687-NGMIAM. Arch Pathol Lab Med. 2006. PMID: 17076533 Review.
Cited by
-
Acute Promyelocytic Leukemia-like AML: Genetic Perspective and Clinical Implications.Cancers (Basel). 2024 Dec 16;16(24):4192. doi: 10.3390/cancers16244192. Cancers (Basel). 2024. PMID: 39766091 Free PMC article. Review.
References
-
- Khoury J.D., Solary E., Abla O., Akkari Y., Alaggio R., Apperley J.F., Bejar R., Berti E., Busque L., Chan J.K.C., et al. The 5th edition of the World Health Organization Classification of Haematolymphoid Tumours: Myeloid and Histiocytic/Dendritic Neoplasms. Leukemia. 2022;36:1703–1719. doi: 10.1038/s41375-022-01613-1. - DOI - PMC - PubMed
-
- Zhao D., Zarif M., Eladl E., Capo-Chichi J.M., Smith A.C., Atenafu E.G., Tierens A., Minden M.D., Schuh A., Chang H. NPM1-mutated AML-MRC diagnosed on the basis of history of MDS or MDS/MPN frequently harbours secondary-type mutations and confers inferior outcome compared to AML with mutated NPM1. Leuk. Res. 2022;118:106869. doi: 10.1016/j.leukres.2022.106869. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

