Optic Nerve Glioblastoma with Optic Chiasm Involvement: A Case Report and a Brief Literature Review
- PMID: 39459474
- PMCID: PMC11509173
- DOI: 10.3390/medicina60101687
Optic Nerve Glioblastoma with Optic Chiasm Involvement: A Case Report and a Brief Literature Review
Abstract
Background: optic nerve glioblastoma is an uncommon pathology. The optic chiasm, optic tract, or optic nerves are possible places from which the tumor can originate. Most of the neuroimaging findings are nonspecific. To confirm the diagnosis, a biopsy is required. A delay to the treatment plan for optic nerve glioblastoma results in poor patient survival rates. Case report: a 68-year-old woman with an uncomplicated medical history presented with exophthalmos, deteriorating eyesight, and partial loss of vision. Using radiological data together with postoperative histopathological and histochemical analysis, optic nerve glioblastoma, IDH-wildtype, with optic chiasm involvement was diagnosed. Conclusion: optic nerve glioblastoma is a rare and aggressive form of cancer that affects the optic nerve, leading to significant vision impairment and potentially life-threatening complications. Treatment options are restricted and difficult because of the location and nature of the condition; surgery, radiation therapy, and chemotherapy are frequently needed as part of a multidisciplinary approach.
Keywords: neurosurgery; ophthalmology; optic nerve glioblastoma; radiology.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


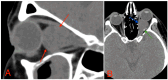





References
-
- Louis D.N., Perry A., Wesseling P., Brat D.J., Cree I.A., Figarella-Branger D., Hawkins C., Ng H.K., Pfister S.M., Reifenberger G., et al. The 2021 WHO Classification of Tumors of the Central Nervous System: A Summary. Neuro. Oncol. 2021;23:1231–1251. doi: 10.1093/neuonc/noab106. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

