West Nile virus can be transmitted within mosquito populations through infectious mosquito excreta
- PMID: 39473977
- PMCID: PMC11513527
- DOI: 10.1016/j.isci.2024.111099
West Nile virus can be transmitted within mosquito populations through infectious mosquito excreta
Abstract
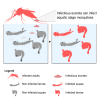
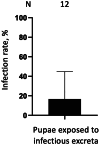
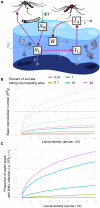
Understanding the transmission routes of arboviruses is key to determining their epidemiology. Here, we tested whether West Nile viruses (WNVs) are transmitted through mosquito excreta. First, we observed a high concentration of infectious units per excreta, although viruses were short lived. Second, we showed that virion excretion starts early after oral infection and remains constant for a long period, regardless of mosquito infection level. These results highlight the infectiousness of excreta from infected mosquitoes. Third, we found that both larvae and pupae were susceptible to infection, while pupae were highly permissive. Fourth, we established the proof-of-concept that immature mosquitoes can be infected by infectious excreta, demonstrating an excreta-mediated mode of transmission. Finally, by mathematically modeling excreta-mediated transmission in the field, we demonstrated that WNV can be transmitted within mosquito populations. Our study uncovers a route of transmission for mosquito-borne arboviruses, unveiling mechanisms of viral maintenance in mosquito reservoirs.
Keywords: disease; pathogenic organism; tropical medicine.
© 2024 The Author(s). Published by Elsevier Inc.
Conflict of interest statement
The authors declare no competing interests.
Figures



References
-
- Heidecke J., Lavarello Schettini A., Rocklöv J. West Nile virus eco-epidemiology and climate change. PLOS Clim. 2023;2 doi: 10.1371/journal.pclm.0000129. - DOI
-
- Smithburn K.C., Hughes T.P., Burke A.W., Paul J.H. A Neurotropic Virus Isolated from the Blood of a Native of Uganda. Am. J. Trop. Med. Hyg. 1940;s1–20:471–492. doi: 10.4269/ajtmh.1940.s1-20.471. - DOI
LinkOut - more resources
Full Text Sources

