Vital Predictive and Prognostic Roles of Triglyceride-Glucose Index in Women With Acute Myocardial Infarction: A Retrospective Cohort Study
- PMID: 39474338
- PMCID: PMC11513407
- DOI: 10.1002/hsr2.70157
Vital Predictive and Prognostic Roles of Triglyceride-Glucose Index in Women With Acute Myocardial Infarction: A Retrospective Cohort Study
Abstract
Background and aims: As a biomarker of insulin resistance (IR) in patients with acute myocardial infarction (AMI), the triglyceride-glucose index (TyG index) has received significant attention. However, most research on AMI has focused on male patients, as it is traditionally believed to primarily affect males. Therefore, this study was conducted on a female population with AMI to investigate the potential correlation between the TyG index and their outcomes.
Methods: A total of 320 women who were admitted to Fujian Provincial Hospital for AMI between January 2017 and December 2019 were included in this study. The TyG index was calculated using the following formula: ln [fasting triglycerides (TG) (mg/dL) × fasting plasma glucose (FPG) (mg/dL)/2]. The primary endpoint of the study was the occurrence of major adverse cardiovascular and cerebrovascular events (MACCEs), which included all-cause mortality, myocardial infarction, repeat revascularization, rehospitalization for heart failure and stroke. The association between the TyG index and unfavorable outcomes in female patients was investigated using the Cox proportional hazards regression model.
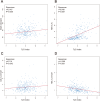
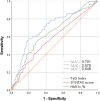
Results: It was ultimately estimated that 111 patients developed MACCEs. Females with high TyG indices had a higher prevalence of diabetes, elevated heart rates, and hemoglobin A1c, as well as a higher likelihood of undergoing thrombus aspiration and stent placement. The TyG index was found to be positively correlated with the prevalence of hypertension, diabetes, low-density lipoprotein cholesterol, hemoglobin A1c, and damaged vessels. However, this correlation was modest, yet statistically significant. Furthermore, after adjusting for conventional risk factors, the TyG index (HR: 4.292, 95% CI: 2.784-6.616, p < 0.001) was independently associated with MACCEs.
Conclusion: As an independent risk predictor, the TyG index has the potential to enhance clinical outcomes for women with AMI.
Keywords: acute myocardial infarction (AMI); female; insulin resistance (IR); major adverse cardiac and cerebral events (MACCEs); triglyceride‐glucose index (TyG index).
© 2024 The Author(s). Health Science Reports published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures





References
-
- Tsao C. W., Aday A. W., Almarzooq Z. I., et al., “Heart Disease and Stroke Statistics‐2022 Update: A Report From the American Heart Association,” Circulation 145, no. 8 (February 2022): e153–e639. - PubMed
-
- Writing Committee of the Report on Cardiovascular Health and Diseases in China , “Report on Cardiovascular Health and Diseases in China 2021: An Updated Summary,” Biomedical and Environmental Sciences 35, no. 7 (2022): 573–603. - PubMed
-
- Mehta L. S., Beckie T. M., DeVon H. A., et al., “Acute Myocardial Infarction in Women: A Scientific Statement From the American Heart Association,” Circulation 133, no. 9 (March 2016): 916–947. - PubMed
-
- Laakso M. and Kuusisto J., “Insulin Resistance and Hyperglycaemia in Cardiovascular Disease Development,” Nature Reviews Endocrinology 10, no. 5 (May 2014): 293–302. - PubMed
-
- Adeva‐Andany M. M., Martínez‐Rodríguez J., González‐Lucán M., Fernández‐Fernández C., and Castro‐Quintela E., “Insulin Resistance Is a Cardiovascular Risk Factor in Humans,” Diabetes & Metabolic Syndrome: Clinical Research & Reviews 13, no. 2 (April 2019): 1449–1455. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

