Ectopic expression of the mitochondrial protein COXFA4L3 in human sperm acrosome and its potential application in the selection of male infertility treatments
- PMID: 39478730
- PMCID: PMC11522028
- DOI: 10.1002/rmb2.12602
Ectopic expression of the mitochondrial protein COXFA4L3 in human sperm acrosome and its potential application in the selection of male infertility treatments
Abstract
Purpose: Spermatogenesis requires a large amount of energy, which is primarily produced by the mitochondrial electron transfer chain. Mitochondrial dysfunction affects male infertility, suggesting a relationship between the electron transfer chain and male infertility. COXFA4L3 (C15ORF48) is an emerging subunit protein of cytochrome oxidase specifically expressed in germ cells during spermatogenesis, and it may be involved in male infertility. Therefore, to investigate whether COXFA4L3 could be a marker of mitochondrial dysfunction in the sperm, this study examined the protein expression and localization profile of COXFA4L3 in the sperm of male patients with infertility.
Methods: Twenty-seven semen samples from a male infertility clinic at the Reproductive Center of Yokohama City University Medical Center were used to analyze sperm quality parameters and the expression and localization of energy production-related proteins. These data were compared with the outcomes of infertility treatment.
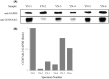
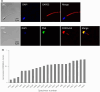
Results: The expression levels of COXFA4L3 varied significantly between samples. Furthermore, COXFA4L3 was ectopically localized to the acrosome.
Conclusions: Ectopic expression of COXFA4L3 and PNA-stained acrosomes may be useful parameters for fertility treatment selection. Assessing the acrosomal localization of COXFA4L3 will expedite pregnancy treatment planning.
Keywords: cytochrome c oxidase; electron transport chain; male infertility; mitochondria; sperm.
© 2024 The Author(s). Reproductive Medicine and Biology published by John Wiley & Sons Australia, Ltd on behalf of Japan Society for Reproductive Medicine.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
Coxfa4l3, a novel mitochondrial electron transport chain Complex 4 subunit protein, switches from Coxfa4 during spermatogenesis.Mitochondrion. 2020 May;52:1-7. doi: 10.1016/j.mito.2020.02.003. Epub 2020 Feb 8. Mitochondrion. 2020. PMID: 32045714
-
Systematic characterization of human testis-specific actin capping protein β3 as a possible biomarker for male infertility.Hum Reprod. 2017 Mar 1;32(3):514-522. doi: 10.1093/humrep/dew353. Hum Reprod. 2017. PMID: 28104696
-
Abnormal fertility, acrosome formation, IFT20 expression and localization in conditional Gmap210 knockout mice.Am J Physiol Cell Physiol. 2020 Jan 1;318(1):C174-C190. doi: 10.1152/ajpcell.00517.2018. Epub 2019 Oct 2. Am J Physiol Cell Physiol. 2020. PMID: 31577511 Free PMC article.
-
A narrative review of mitochondrial dysfunction and male infertility.Transl Androl Urol. 2024 Sep 30;13(9):2134-2145. doi: 10.21037/tau-24-262. Epub 2024 Sep 26. Transl Androl Urol. 2024. PMID: 39434760 Free PMC article. Review.
-
Causes and consequences of sperm mitochondrial dysfunction.Andrologia. 2021 Feb;53(1):e13666. doi: 10.1111/and.13666. Epub 2020 Jun 8. Andrologia. 2021. PMID: 32510691 Review.
Cited by
-
Protein profile of spermatozoa and seminal plasma based on molecular weight in four phenotypes of Kokok Balenggek roosters.Open Vet J. 2025 Mar;15(3):1322-1330. doi: 10.5455/OVJ.2025.v15.i3.23. Epub 2025 Mar 31. Open Vet J. 2025. PMID: 40276196 Free PMC article.
References
-
- WHO laboratory manual for the examination and processing of human semen. 6th ed. Geneva: World Health Organization; 2021. License: CC BY‐NC‐SA 3.0 IGO.
LinkOut - more resources
Full Text Sources
