Safety and early efficacy of involved-field SBRT for nodal oligo-recurrent prostate cancer
- PMID: 39484030
- PMCID: PMC11524995
- DOI: 10.3389/fonc.2024.1434504
Safety and early efficacy of involved-field SBRT for nodal oligo-recurrent prostate cancer
Abstract
Purpose: Following treatment for localized prostate cancer, a subset of men will develop recurrent disease in the abdominopelvic nodes. For radiation therapy (RT), the optimal treatment volume, fractionation schedule, and dose remain unanswered questions. We report early outcomes for patients treated with involved-field stereotactic body radiation therapy (SBRT) (IF-SBRT) for nodal oligo-recurrent (NOR) prostate cancer.
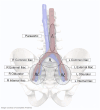
Methods: Between January 2018 and October 2023, 67 patients with a median age of 75 with NOR prostate cancer treated with 74 courses of IF-SBRT at Georgetown were eligible for this analysis. NOR was defined as any volume of disease that could be safely treated within an IF. All patients were treated with five-fraction IF-SBRT (27.5-35 Gy). The IF treatment volume was defined as the nodal basin containing the gross disease as well as the immediately adjacent basins. Disease progression was defined as a prostate-specific antigen (PSA) rise above the pretreatment baseline or initiation of a second treatment. Local control and progression-free survival were calculated using the Kaplan-Meier method.
Results: Detection of pre-SBRT NOR was ascertained by prostate-specific membrane antigen (PSMA) (38%), fluciclovine (50%), or MRI/CT (12%). Median follow-up was 50 months (1-262). The median pre-salvage PSA was 6.5 ng/mL (range, 0.1-335). The median number of involved nodes was 3 (range, 1-16). The local control at 1 and 2 years was 98% and 93%, respectively. The 1- and 2-year progression-free survival was 78% and 50%, respectively. Twenty percent of treatment courses were followed by acute Grade 2 gastrointestinal (GI) toxicity: diarrhea (9%) and/or nausea (14%). Two patients (3%) experienced late Grade 2 nausea. On univariate analysis, measures of disease volume such as hormone sensitivity (p = 0.03), increasing involved node number (p = 0.008), and abdominal treatment (p = 0.03) were significantly associated with GI toxicity.
Conclusions: With the widespread adoption of PSMA agents, NORs are likely to increase. The optimal combination of local and systemic therapy in this population is unknown. With a favorable toxicity profile, IF-SBRT represents a safe and convenient local therapy treatment option for an elderly patient population. Patient- and treatment-related factors such as a large number of involved nodes and/or abdominal treatment may be associated with an increased risk of GI toxicity.
Keywords: CyberKnife; SBRT; common toxicity criteria (CTC); involved field; nodal oligo-recurrence; prostate cancer.
Copyright © 2024 Koh, Pilkington, Koh, Lawlor, Creswell, O’Connor, Zwart, Danner, Kumar, Suy, Carrasquilla and Collins.
Conflict of interest statement
SC serves as a clinical consultant to Accuray, Inc., Blue Earth Diagnostics, Pfizer, and Sumitomo Pharma America, Inc. The Department of Radiation Medicine at Georgetown University Hospital receives a grant from Accuray to support a research coordinator. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The author(s) declared that they were an editorial board member of Frontiers, at the time of submission. This had no impact on the peer review process and the final decision.
Figures
References
-
- Carrasquilla M, Creswell ML, Pepin AN, Wang E, Forsthoefel M, McGunigal M, et al. Rationale for involved field stereotactic body radiation therapy-enhanced intermittent androgen deprivation therapy in hormone-sensitive nodal oligo-recurrent prostate cancer following prostate stereotactic body radiation therapy. Front Oncol. (2021) 10:606260. doi: 10.3389/fonc.2020.606260 - DOI - PMC - PubMed
-
- Messing EM, Manola J, Yao J, Kiernan M, Crawford D, Wilding G, et al. Immediate versus deferred androgen deprivation treatment in patients with node-positive prostate cancer after radical prostatectomy and pelvic lymphadenectomy. Lancet Oncol. (2006) 7:472–9. doi: 10.1016/S1470-2045(06)70700-8 - DOI - PubMed
-
- Miszczyk M, Rajwa P, Yanagisawa T, Nowicka Z, Shim SR, Laukhtina E, et al. The efficacy and safety of metastasis-directed therapy in patients with prostate cancer: A systematic review and meta-analysis of prospective studies. Eur Urol. (2024) 85:125–38. doi: 10.1016/j.eururo.2023.10.012 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

