Improvement of the outcome of the saphenous vein graft when connected to the internal thoracic artery
- PMID: 39494236
- PMCID: PMC11527685
- DOI: 10.3389/fcvm.2024.1478166
Improvement of the outcome of the saphenous vein graft when connected to the internal thoracic artery
Abstract
Background: Since 2000, we have been grafting the right coronary artery system (RCAs) using the proximal portion of the right internal thoracic artery (RITA) as the inflow of the saphenous vein graft (SVG) to increase the number of patients undergoing beating heart complete myocardial revascularization.
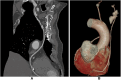
Methods: From 2000 to 2022, 928 consecutive patients underwent SVG on the RCAs. In 546 patients (58.8%), the inflow was the RITA (I-graft group), and in 382 patients (41.2%), the inflow was the aorta (Ao-graft group). The inclusion criteria were age ≤75 years, ejection fraction >35%, only one SVG per patient, bilateral internal thoracic arteries as a Y-graft on the left system (three-vessel disease, n = 817, 88.0%) or left internal thoracic artery on the left anterior descending artery and RITA + SVG on the RCAs (two-vessel disease, n = 111, 12.0%). Propensity matching identified 306 patients per group. After a median follow-up of 8 (5-10) years, graft patency was assessed by coronary computed tomographic angiography in 132 patients (64 in the I-graft group and 68 in the Ao-graft group).
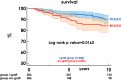
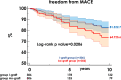
Results: Early results were similar in both groups. The I-graft group had higher 10-year survival and freedom from main adverse cardiac events (90.0 ± 2.0 vs. 80.6 ± 3.8, p = 0.0162, and 81.3 ± 2.7 vs. 64.7 ± 5.6, p = 0.0206, respectively). When RITA was the inflow, SVG had a higher estimated 10-year patency rate (82.8% ± 6.5 vs. 58.8% ± 7.4, p = 0.0026) and a smaller inner lumen diameter (2.7 ± 0.4 vs. 3.4 ± 0.6 mm, p < 0.0001).
Conclusion: When the inflow is the RITA, SVG grafted to the RCAs (I-graft) may result in a higher patency rate and better outcome than when the inflow is the ascending aorta (Ao-graft). The continuous supply of nitric oxide by RITA may be the cause of the higher patency rate of the I-graft, which can behave like an arterial conduit.
Keywords: I-graft; OPCAB; anaortic bypass; composite graft; saphenous vein graft.
© 2024 Katsavrias, Prapas, Calafiore, Taggart, Angouras, Iliopoulos, Di Mauro, Papandreopoulos, Zografos and Dougenis.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Saphenous vein to the right coronary system from the right thoracic artery or the aorta. Long-term propensity-matched results of 2 groups.Eur J Cardiothorac Surg. 2024 Mar 1;65(3):ezae060. doi: 10.1093/ejcts/ezae060. Eur J Cardiothorac Surg. 2024. PMID: 38400814
-
Revascularization for the right coronary artery territory in off-pump coronary artery bypass surgery.Ann Thorac Surg. 2013 Sep;96(3):778-85; discussion 785. doi: 10.1016/j.athoracsur.2013.04.097. Epub 2013 Jul 16. Ann Thorac Surg. 2013. PMID: 23866806
-
V-composite grafting using the right internal thoracic artery grafts anastomosed to aorto-coronary bypass grafts.Eur J Cardiothorac Surg. 2015 Nov;48(5):753-7. doi: 10.1093/ejcts/ezu525. Epub 2015 Jan 18. Eur J Cardiothorac Surg. 2015. PMID: 25602057
-
Equipoise between radial artery and right internal thoracic artery as the second arterial conduit in left internal thoracic artery-based coronary artery bypass graft surgery: a multi-institutional study†.Eur J Cardiothorac Surg. 2016 Jan;49(1):188-95. doi: 10.1093/ejcts/ezv093. Epub 2015 Mar 11. Eur J Cardiothorac Surg. 2016. PMID: 25762396
-
Does the right internal thoracic artery or saphenous vein graft offer superior revascularization of the right coronary artery?Interact Cardiovasc Thorac Surg. 2012 Aug;15(2):244-7. doi: 10.1093/icvts/ivs180. Epub 2012 May 3. Interact Cardiovasc Thorac Surg. 2012. PMID: 22561293 Free PMC article. Review.
References
-
- Gaudino M, Di Franco A, Rahouma M, Tam DY, Iannaccone M, Deb S, et al. Unmeasured confounders in observational studies comparing bilateral versus single internal thoracic artery for coronary artery bypass grafting: a meta-analysis. J Am Med Assoc. (2018) 7:e008010. 10.1161/JAHA.117.008010 - DOI - PMC - PubMed
-
- Samano N, Geijer H, Liden M, Fremes S, Bodin L, Souza D. The no-touch saphenous vein for coronary artery bypass grafting maintains a patency, after 16 years, comparable to the left internal thoracic artery: a randomized trial. J Thorac Cardiovasc Surg. (2015) 150:880–8. 10.1016/j.jtcvs.2015.07.027 - DOI - PubMed
LinkOut - more resources
Full Text Sources

