Relationship between lactate levels and 28-day mortality in pediatric sepsis: results from the pediatric intensive care database
- PMID: 39511557
- PMCID: PMC11542395
- DOI: 10.1186/s12887-024-05200-4
Relationship between lactate levels and 28-day mortality in pediatric sepsis: results from the pediatric intensive care database
Abstract
Objective: This study aimed to investigate the relationship between serum lactate levels at admission to the intensive care unit (ICU) and the clinical outcomes of children with sepsis.
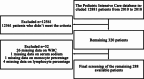
Methods: We used the Pediatric Intensive Care (PIC) database to identify 288 pediatric patients with sepsis. We analyzed the relationship between lactate levels and hospital and ICU mortality in sepsis by establishing a segmented multivariable Cox regression model. We also conducted subgroup analysis as well as analyzed the restricted cubic spline curves.
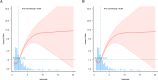
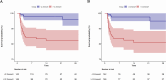
Results: After adjusting for all potential confounding factors, an increase of 1 mmol/L in lactate levels was found to be associated with an 17% rise in the 28-day hospital mortality risk among sepsis patients (HR: 1.17, 95% CI: 1.08-1.27, P = 0.0002). When considering lactate as a categorical variable, the mortality risk of patients with lactate levels ≥ 2.2 mmol/L was significantly increased (HR: 3.61, 95% CI: 1.24-10.54, P = 0.0189). The restricted cubic spline curve analysis revealed a nonlinear correlation between lactate and 28-day mortality, with an inflection point at 2.2 mmol/L. Similar findings were also observed in the assessment of secondary outcomes.
Conclusions: Our study demonstrates a non-linear correlation between lactate levels and 28-day mortality in pediatric sepsis, with a critical threshold of 2.2mmol/l for lactate levels in septic patients. Early assessment of lactate levels is recommended for children with sepsis to facilitate prompt intervention and mitigate the risk of fatality.
Keywords: Lactate; Mortality; PIC database; Pediatrics; Sepsis.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
Evaluation of the Association of Early Elevated Lactate With Outcomes in Children With Severe Sepsis or Septic Shock.Pediatr Emerg Care. 2019 Oct;35(10):661-665. doi: 10.1097/PEC.0000000000001021. Pediatr Emerg Care. 2019. PMID: 28072671 Free PMC article.
-
A retrospective study utilized MIMIC-IV database to explore the potential association between triglyceride-glucose index and mortality in critically ill patients with sepsis.Sci Rep. 2024 Oct 15;14(1):24081. doi: 10.1038/s41598-024-75050-8. Sci Rep. 2024. PMID: 39402158 Free PMC article.
-
Blood Lactate Levels Cutoff and Mortality Prediction in Sepsis-Time for a Reappraisal? a Retrospective Cohort Study.Shock. 2016 Nov;46(5):480-485. doi: 10.1097/SHK.0000000000000667. Shock. 2016. PMID: 27380535 Free PMC article.
-
Prediction of pediatric sepsis mortality within 1 h of intensive care admission.Intensive Care Med. 2017 Aug;43(8):1085-1096. doi: 10.1007/s00134-017-4701-8. Epub 2017 Feb 20. Intensive Care Med. 2017. PMID: 28220227
-
Lactate, an Essential Metabolic Marker in the Diagnosis and Management of Pediatric Conditions.Diagnostics (Basel). 2025 Mar 23;15(7):816. doi: 10.3390/diagnostics15070816. Diagnostics (Basel). 2025. PMID: 40218166 Free PMC article. Review.
Cited by
-
Relationship between preoperative high arterial blood lactate level and delirium after deep brain stimulation surgery in Parkinson's disease.Front Aging. 2025 Mar 25;6:1538012. doi: 10.3389/fragi.2025.1538012. eCollection 2025. Front Aging. 2025. PMID: 40201747 Free PMC article.
References
-
- Cecconi M, Evans L, Levy M, Rhodes A. Sepsis and septic shock. Lancet. 2018;392(10141):75–87. - PubMed
-
- Santiago CD, Menezes AM, de Carvalho WB, Delgado AF. Epidemiologic challenges in sepsis to the developing countries. Pediatr Crit Care Med. 2013;14(3):336. - PubMed
-
- Fleischmann-Struzek C, Goldfarb DM, Schlattmann P, Schlapbach LJ, Reinhart K, Kissoon N. The global burden of paediatric and neonatal sepsis: a systematic review. Lancet Respir Med. 2018;6(3):223–30. - PubMed
-
- Fleischmann C, Scherag A, Adhikari NK, Hartog CS, Tsaganos T, Schlattmann P, et al. Assessment of Global Incidence and Mortality of Hospital-treated Sepsis. Current estimates and limitations. Am J Respir Crit Care Med. 2016;193(3):259–72. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

