Novel Expression of Apical Bile Acid Transport (ASBT) More Proximally Than Distal Ileum Contributing to Enhanced Intestinal Bile Acid Absorption in Obesity
- PMID: 39519005
- PMCID: PMC11547122
- DOI: 10.3390/ijms252111452
Novel Expression of Apical Bile Acid Transport (ASBT) More Proximally Than Distal Ileum Contributing to Enhanced Intestinal Bile Acid Absorption in Obesity
Abstract
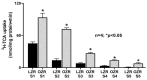
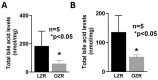
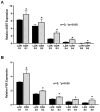
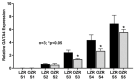
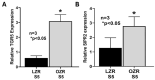
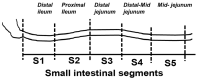
Dietary lipid absorption is facilitated by bile acids. In the Zucker rat (ZR) model of obesity, bile acid absorption, mediated by the apical sodium bile acid transporter (ASBT), was increased in villus cells from the distal ileum. However, whether ASBT may be de novo expressed more proximally in the small intestine during obesity to facilitate additional bile acid absorption is not known. For this, starting from the end of the ileum to the mid jejunum, caudal-orally, five intestinal segments of equal length (S1-S5) were separated from lean and obese ZRs (LZR and OZR). Intestinal mucosa obtained from these segments were used for total RNA extraction, RT-qPCR and 3H-TCA uptake. The results showed that bile acid absorption along with the mRNA expression of ASBT and FXR progressively decreased caudal-orally in both LZRs and OZRs but was significantly higher in all small intestinal segments in OZRs. The expression of GATA4 was absent in the distal ileum (S1) in both LZRs and OZRs, but steadily increased along the proximal length in both. However, this steady increase was significantly reduced in the comparative obese proximal intestinal segments S2, S3, S4 and S5. The expressions of bile acid-activated G-protein-coupled bile acid receptor TGR5 and S1PR2 were unaltered in segments S1-S4 but were significantly increased in OZR S5. The paradigm changing observation of this study is that ASBT is expressed more proximally in the small intestine in obesity. This likely increases overall bile acid absorption and thereby lipid absorption in the proximal small intestine in obesity.
Keywords: apical sodium bile acid transporter; bile acids; farnesoid X receptor; intestinal physiology; metabolic disorders; obesity; obesity-related risk factors.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Mechanism of Dyslipidemia in Obesity-Unique Regulation of Ileal Villus Cell Brush Border Membrane Sodium-Bile Acid Cotransport.Cells. 2019 Oct 3;8(10):1197. doi: 10.3390/cells8101197. Cells. 2019. PMID: 31623375 Free PMC article.
-
Expression of Bile Acid Receptors and Transporters Along the Intestine of Patients With Type 2 Diabetes and Controls.J Clin Endocrinol Metab. 2025 Feb 18;110(3):e660-e666. doi: 10.1210/clinem/dgae261. J Clin Endocrinol Metab. 2025. PMID: 38636096
-
Weanling, but not adult, rabbit colon absorbs bile acids: flux is linked to expression of putative bile acid transporters.Am J Physiol Gastrointest Liver Physiol. 2006 Mar;290(3):G439-50. doi: 10.1152/ajpgi.00163.2005. Epub 2005 Sep 15. Am J Physiol Gastrointest Liver Physiol. 2006. PMID: 16166347
-
Intestinal bile acid transport: biology, physiology, and pathophysiology.J Pediatr Gastroenterol Nutr. 2001 Apr;32(4):407-17. doi: 10.1097/00005176-200104000-00002. J Pediatr Gastroenterol Nutr. 2001. PMID: 11396803 Review.
-
Role of the intestinal bile acid transporters in bile acid and drug disposition.Handb Exp Pharmacol. 2011;(201):169-203. doi: 10.1007/978-3-642-14541-4_4. Handb Exp Pharmacol. 2011. PMID: 21103970 Free PMC article. Review.
References
-
- Angkurawaranon C., Wisetborisut A., Rerkasem K., Seubsman S.A., Sleigh A., Doyle P., Nitsch D. Early life urban exposure as a risk factor for developing obesity and impaired fasting glucose in later adulthood: Results from two cohorts in Thailand. BMC Public Health. 2015;15:902. doi: 10.1186/s12889-015-2220-5. - DOI - PMC - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

