Natural History and Microbiological Profiles of Patients With Acute Pancreatitis With Suspected Infected Pancreatic Necrosis
- PMID: 39525090
- PMCID: PMC11550862
- DOI: 10.7759/cureus.71853
Natural History and Microbiological Profiles of Patients With Acute Pancreatitis With Suspected Infected Pancreatic Necrosis
Abstract
Introduction: Acute pancreatitis (AP) is a prevalent emergency. The clinical spectrum of the condition is varied, ranging from a mild to a malignant course with higher mortality rates. Infection of pancreatic/peri necrosis, extrapancreatic infections, and organ failure are significant complications in AP. In the recent era, microbiological composition has shifted more towards multi-drug-resistant organisms due to irrational antibiotic use.
Objective: This study aims to understand the natural history of patients with suspected infected pancreatic necrosis (IPN), the prevalence of multi-drug-resistant organisms (MDROs), and their antibiotic susceptibility patterns.
Methods: This prospective, observational study was performed on 130 cases of acute necrotizing pancreatitis (ANP) with suspected IPN that were evaluated during their period of admission in the department of gastroenterology, emergency medicine, or surgery ward of the Postgraduate Institute of Medical Education and Research, Chandigarh, India, a tertiary hospital. The details of outcomes were recorded. The organisms in cases with IPN and antibiotic resistance patterns of various organisms were studied.
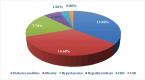
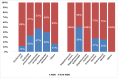
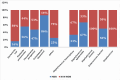
Results: The most prevalent site of necrosis was combined pancreatic and peripancreatic tissues in 111 (85.4%) patients. The computed tomography severity index (CTSI) had a mean of 8.72±1.43. Of all participants, 36 (27.7%) patients had <30% necrosis, 47 (36.2%) had 30%-50% necrosis, and 47 (36.2%) had >50% necrosis. Overall, 80 (61.5%) patients had organ failure, with acute lung injury (ALI) being the most common. Rates of complications were markedly greater in cases with higher pancreatic necrosis and with infected necrosis (p<0.05). The most common organism isolated from necrotic tissue was Escherichia coli (E. coli) in 17 (32.07%) cases, followed by Acinetobacter baumannii (A. baumannii) in 12 (22.64%) cases. The most common extrapancreatic infection site was respiratory tract infections. Pseudomonas aeruginosa (P. aeruginosa) and A. baumannii revealed maximum resistance to most of the drugs. Conclusion: Infected pancreatic necrosis is linked to high rates of morbidity and mortality. Our study suggests that irrational usage of antibiotics increases the incidence of combined infection, especially with higher rates of multi-drug-resistant infections.
Keywords: acute pancreatitis; extrapancreatic infection; gram-negative bacteria; infected pancreatic necrosis; microbiological profile in pancreatitis; multi-drug resistance; organ failure.
Copyright © 2024, Loganathan et al.
Conflict of interest statement
Human subjects: Consent was obtained or waived by all participants in this study. Institutional Ethics Committee, Postgraduate Institute of Medical Education and Research issued approval (NK/6218/MD/725). Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures

References
-
- Global incidence and mortality of pancreatic diseases: a systematic review, meta-analysis, and meta-regression of population-based cohort studies. Xiao AY, Tan ML, Wu LM, Asrani VM, Windsor JA, Yadav D, Petrov MS. Lancet Gastroenterol Hepatol. 2016;1:45–55. - PubMed
-
- Comparison of procalcitonin and C-reactive protein as markers of sepsis. Luzzani A, Polati E, Dorizzi R, Rungatscher A, Pavan R, Merlini A. Crit Care Med. 2003;31:1737–1741. - PubMed
-
- Classification of acute pancreatitis-2012: revision of the Atlanta classification and definitions by international consensus. Banks PA, Bollen TL, Dervenis C, et al. Gut. 2013;62:102–111. - PubMed
-
- Acute pancreatitis: recent advances through randomised trials. van Dijk SM, Hallensleben ND, van Santvoort HC, Fockens P, van Goor H, Bruno MJ, Besselink MG. Gut. 2017;66:2024–2032. - PubMed
LinkOut - more resources
Full Text Sources
