Mildly elevated serum prolactin level may be a protective factor for preventing thickening of the carotid intima-media in patients with type 2 diabetes mellitus
- PMID: 39526908
- PMCID: PMC11728874
- DOI: 10.1530/EC-24-0285
Mildly elevated serum prolactin level may be a protective factor for preventing thickening of the carotid intima-media in patients with type 2 diabetes mellitus
Abstract
Objective: To evaluate the correlation between the serum prolactin (PRL) level and carotid intima-media thickness (CIMT) in patients with type 2 diabetes mellitus (T2DM).
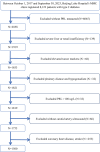
Methods: In this study, 1,500 participants were divided into three groups based on the serum PRL level: hypoprolactinemia group (PRL ≤ 7 μg/L), normal PRL level group (7 μg/L < PRL ≤ 25 μg/L), and homeostatic functionally increased transient PRL (Ho-PRL) group (25 μg/L < PRL ≤ 100 μg/L). The independent-sample Kruskal-Wallis test was used to compare the CIMT among the three groups. The Spearman correlation test was used to examine the relationship between the CIMT, serum PRL level, and clinical data. Multivariate linear regression analysis was used to determine the independent factors that influence the CIMT.
Result: Individuals in the Ho-PRL group had a significantly lower CIMT compared to the hypoprolactinemia and normal PRL level groups (P < 0.001). The CIMT was positively correlated with age, systolic blood pressure (SBP), body mass index, duration of T2DM, and luteinizing hormone and follicle-stimulating hormone levels and negatively correlated with alanine transaminase and aspartate transaminase activities, estimated glomerular filtration rate, and PRL. Multivariate linear regression analysis revealed that only PRL was negatively associated with the CIMT, while age and SBP were positively associated with the CIMT.
Conclusion: In patients with T2DM, a PRL level within the mildly elevated range is negatively correlated with the CIMT. A mildly elevated serum PRL level may be a protective factor for preventing thickening of the carotid intima-media.
Keywords: carotid intima-media thickness; homeostatic functionally increased transient PRL; prolactin; type 2 diabetes.
Conflict of interest statement
The authors declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the work.
Figures

Similar articles
-
Association Between Serum Uric Acid and Carotid Intima-Media Thickness in Different Fasting Blood Glucose Patterns: A Case-Control Study.Front Endocrinol (Lausanne). 2022 May 27;13:899241. doi: 10.3389/fendo.2022.899241. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 35712254 Free PMC article.
-
The possible correlation between serum GRB2 levels and carotid atherosclerosis in patients with type 2 diabetes mellitus.Front Endocrinol (Lausanne). 2022 Sep 13;13:963191. doi: 10.3389/fendo.2022.963191. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 36176460 Free PMC article.
-
Association of Estimated GFR (By MDRD) with the Carotid Intima Media Thickness (CIMT) in Different Stages of CKD among Patients with Type 2 Diabetes Mellitus.Mymensingh Med J. 2020 Jan;29(1):209-214. Mymensingh Med J. 2020. PMID: 31915360
-
Meta-analysis of the correlation between serum uric acid level and carotid intima-media thickness.PLoS One. 2021 Feb 11;16(2):e0246416. doi: 10.1371/journal.pone.0246416. eCollection 2021. PLoS One. 2021. PMID: 33571245 Free PMC article.
-
Systematic review and meta-analysis assessing the status of carotid intima-media thickness and lipid profiles in type 2 diabetes mellitus.BMJ Open. 2024 Nov 9;14(11):e087496. doi: 10.1136/bmjopen-2024-087496. BMJ Open. 2024. PMID: 39521468 Free PMC article.
Cited by
-
Association between serum bilirubin levels and carotid atherosclerosis: a systematic review and meta-analysis.Front Endocrinol (Lausanne). 2025 Jun 19;16:1451465. doi: 10.3389/fendo.2025.1451465. eCollection 2025. Front Endocrinol (Lausanne). 2025. PMID: 40612433 Free PMC article.
References
LinkOut - more resources
Full Text Sources

