Drug-induced acute kidney injury: a cohort study on incidence, identification of pathophysiological mechanisms, and prognostic factors
- PMID: 39534223
- PMCID: PMC11554514
- DOI: 10.3389/fmed.2024.1459170
Drug-induced acute kidney injury: a cohort study on incidence, identification of pathophysiological mechanisms, and prognostic factors
Abstract
Introduction: Acute Kidney Injury (AKI) is a common clinical syndrome characterized by an abrupt decline in the glomerular filtration rate (GFR), which can cause severe alterations in blood volume and acid-base balance. Drug-Induced Acute Kidney Injury (DI-AKI) is associated with exposure to nephrotoxic medications, particularly among hospitalized patients. Adverse drug reactions comprises type A and type B reactions. Type A reactions are predictable based on the pharmacology of the substance, dose-dependent, and manifest as Acute Tubular Necrosis (ATN). Type B reactions are unpredictable, idiosyncratic, not dose-dependent, and manifest as Acute Interstitial Nephritis (AIN), Crystal-Induced Nephropathy, among others.
Objective: To evaluate DI-AKI incidence, identify the main associated drugs and the pathophysiological mechanism of the observed injury, analyze prognostic factors associated with unfavorable outcomes, and compare the outcomes of death and the need for Acute Kidney Support Therapy (AKST) between patients with DI-AKI vs. AKI due to other etiologies.
Methods: A retrospective cohort study conducted at the Hospital das Clínicas of the Faculty of Medicine of Botucatu - UNESP (HC-FMB), using data from patients hospitalized between January 2016 and April 2022 and followed, via consultation, by the AKI-Nephrology team. Inclusion criteria: diagnosis of AKI and Chronic Kidney Disease (CKD) with superimposed AKI. Exclusion criteria: patients under 18 years old or on chronic Renal Replacement Therapy. AKI was diagnosed based on creatinine increase as established by KDIGO 2012. Data were presented as mean and standard deviation or median with interquartile range and frequency. Statistical significance was set at 5% (p < 0.05). Comparative analyses were performed using the Chi-Square test for categorical variables and the T-test for continuous variables. Subsequently, logistic regression was performed to identify factors associated with the need for AKST and death.
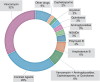
Results: A total of 1,398 patients were analyzed, most of them males (61.4%), with a mean age of 64 years ±14.4 years. The most prevalent etiology of AKI was Mixed Ischemic + Septic AKI (28%). DI-AKI was a significant cause of AKI (19.3%). Of these, 25.2% were isolated DI-AKI and 74.8% were Mixed DI-AKI + Ischemia and/or Sepsis. Among patients with DI-AKI, the mean age was 61.15 ± 15.26, males were the most frequent, the majority were not subjected to AKST and survived. Most of these patients were hospitalized in the ward, did not need vasoactive drugs, nor did they use mechanical ventilation. DI-AKI showed lower severity and mortality compared to other AKI etiologies but had a similar need for AKST (26.3% vs. 35.4%, p < 0.05 and 31.8% vs. 36.8%, p > 0.05). Most nephrotoxic drugs caused type A reactions, with Vancomycin being the primary nephrotoxin. Among drugs associated with DI-AKI, Vancomycin was associated with a higher need for AKST and death, while Amphotericin B was associated with a lower risk of AKST and death.
Conclusion: Although the mortality rate is lower among DI-AKIs compared to other AKI etiologies, the need for AKST was similar. Therefore, it is recommended that DI-AKI be recognized early to enable dose reduction or even drug suspension, depending on the type of reaction, to reduce healthcare costs and improve clinical outcomes for patients.
Keywords: AKI (acute kidney injury); DI-AKI (drug-induced acute kidney injury); incidence; nephrotoxicity; prognosis.
Copyright © 2024 Garcia, Pacchini, Zamoner, Balbi and Ponce.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Clinico-Etiological Spectrum and Outcome in Patients With Septic Acute Kidney Injury and Its Comparison With Non-septic Acute Kidney Injury: A Hospital-Based Prospective Study Conducted in a Tertiary Care Hospital in North India.Cureus. 2023 Apr 19;15(4):e37857. doi: 10.7759/cureus.37857. eCollection 2023 Apr. Cureus. 2023. PMID: 37223179 Free PMC article.
-
Survey of acute kidney injury and related risk factors of mortality in hospitalized patients in a third-level urban hospital of Shanghai.Blood Purif. 2014;38(2):140-8. doi: 10.1159/000366127. Epub 2014 Nov 27. Blood Purif. 2014. PMID: 25471326
-
Early recovery status and outcomes after sepsis-associated acute kidney injury in critically ill patients.Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2022 May 28;47(5):535-545. doi: 10.11817/j.issn.1672-7347.2022.210368. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2022. PMID: 35753723 Free PMC article.
-
AGA Clinical Practice Update on the Evaluation and Management of Acute Kidney Injury in Patients With Cirrhosis: Expert Review.Clin Gastroenterol Hepatol. 2022 Dec;20(12):2707-2716. doi: 10.1016/j.cgh.2022.08.033. Epub 2022 Sep 6. Clin Gastroenterol Hepatol. 2022. PMID: 36075500 Review.
-
Facing the Challenge of Drug-Induced Acute Interstitial Nephritis.Nephron. 2023;147(2):78-90. doi: 10.1159/000525561. Epub 2022 Jul 13. Nephron. 2023. PMID: 35830831 Review.
Cited by
-
Anthraquinones from Rheum officinale Ameliorate Renal Fibrosis in Acute Kidney Injury and Chronic Kidney Disease.Drug Des Devel Ther. 2025 Jul 6;19:5739-5760. doi: 10.2147/DDDT.S521265. eCollection 2025. Drug Des Devel Ther. 2025. PMID: 40657042 Free PMC article. Review.
-
Application of Nanomaterial-Mediated Ferroptosis Regulation in Kidney Disease.Int J Nanomedicine. 2025 Feb 5;20:1637-1659. doi: 10.2147/IJN.S496644. eCollection 2025. Int J Nanomedicine. 2025. PMID: 39931533 Free PMC article. Review.
References
LinkOut - more resources
Full Text Sources
Miscellaneous