Dorsal venous complex ligation-free and parietal endopelvic fascia preserving in laparoscopic radical prostatectomy: A prospective study of single centre
- PMID: 39539566
- PMCID: PMC11557257
- DOI: 10.1002/bco2.437
Dorsal venous complex ligation-free and parietal endopelvic fascia preserving in laparoscopic radical prostatectomy: A prospective study of single centre
Erratum in
-
Erratum.BJUI Compass. 2024 Dec 30;5(12):1324-1329. doi: 10.1002/bco2.482. eCollection 2024 Dec. BJUI Compass. 2024. PMID: 39744071 Free PMC article.
Abstract
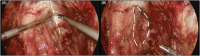
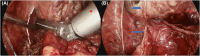
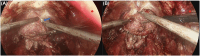
Objectives: This study aims to describe a novel dorsal venous complex (DVC) ligation-free and parietal endopelvic fascia preserving technique for laparoscopic radical prostatectomy and to evaluate its post-operative outcomes.
Methods: From April 2020 to May 2021, a total of 125 patients with localized prostate cancer received laparoscopic radical prostatectomy by a single surgeon. In the procedure, a novel technique of DVC ligation-free and parietal endopelvic fascia preserving was used. Preoperative characteristics of patients and perioperative results were recorded. In this study, continence was defined as zero to one pad per day. Oncological outcomes were evaluated based on positive surgical margin.
Results: Five patients required a blood transfusion. Mean post-operative hospital stay was 3.9 days (2-5), and the catheter could be removed on post-operative day 7 to 9. Final pathologic evaluations were 87 stage pT2, 22 stage pT3a, and 7 pT3b, 9 stage pT4, respectively. The positive surgical margin rate was 10.4% in total. Ninety-three patients (74.4%) returned to urinary continence 2 months post-operatively, and 11 patients (11/125) developed biochemical recurrence 6 months post-operatively.
Conclusions: The DVC ligation-free and parietal endopelvic fascia preserving technique provides early recovery from incontinence without adversely affecting the oncological outcome.
Keywords: dorsal venous complex; endopelvic fascia; parietal; prostate cancer; radical prostatectomy.
© 2024 The Author(s). BJUI Compass published by John Wiley & Sons Ltd on behalf of BJU International Company.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Walz J, Epstein JI, Ganzer R, Graefen M, Guazzoni G, Kaouk J, et al. A critical analysis of the current knowledge of surgical anatomy of the prostate related to optimisation of cancer control and preservation of continence and erection in candidates for radical prostatectomy: an update. Eur. Urol. 2016;70(2):301–311. 10.1016/j.eururo.2016.01.026 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
