Insights into Helicobacter pylori macrolide resistance: a comprehensive systematic review and meta-analysis
- PMID: 39539713
- PMCID: PMC11557415
- DOI: 10.3389/fmicb.2024.1481763
Insights into Helicobacter pylori macrolide resistance: a comprehensive systematic review and meta-analysis
Abstract
Background: Helicobacter pylori infection is a primary global health concern. However, the widespread use of antibiotics, particularly macrolides such as clarithromycin, has increased resistance among H. pylori strains. This study aimed to investigate the prevalence of macrolide resistance in H. pylori in different world regions.
Methods: This systematic literature search was performed using the appropriate search syntax after searching PubMed, Embase, Web of Science, and Scopus databases between May 2015 and December 2023. Statistical analysis was performed using Pooled and random effects model in R and the metafor package.
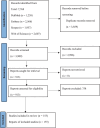
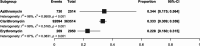
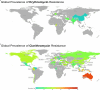
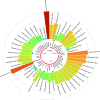
Results: A total of 7,768 articles were retrieved. After a thorough evaluation, 155 studies (by 178 reports) were finally eligible for inclusion in this systematic review and meta-analysis. According to the results, the majority of studies (178 reports from 43 countries) assessed clarithromycin susceptibility, with a pooled prevalence of 33.3% and high heterogeneity between studies (I 2 = 98.57%, p < 0.001). The rate of erythromycin resistance was moderate (22.8%, 10 reports), while azithromycin resistance was 34.4% (4 reports). Subgroup analysis revealed significant differences in the prevalence of resistance based on geographic location, continent, and year of publication. Clarithromycin resistance increased from 29.1% (2015-2019) to 36.5% (2020-2023).
Conclusion: This study highlights the critical challenges of macrolide resistance in treating H. pylori infection. The high prevalence and geographic variation underscore the need for tailored treatment strategies based on regional resistance patterns. Furthermore, continuously monitoring resistance trends and investigating contributing factors are essential to optimize treatment.
Systematic review registration: https://www.crd.york.ac.uk/prospero; CRD42024557749.
Keywords: Helicobacter pylori; antibiotic resistance; azithromycin; clarithromycin; erythromycin; macrolides.
Copyright © 2024 Morad Kasani, Mofid, Navidifar, Golab, Parvizi, Badmasti, Sholeh and Beig.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

Similar articles
-
Insights into Haemophilus macrolide resistance: A comprehensive systematic review and meta-analysis.PLoS Negl Trop Dis. 2025 Mar 4;19(3):e0012878. doi: 10.1371/journal.pntd.0012878. eCollection 2025 Mar. PLoS Negl Trop Dis. 2025. PMID: 40036252 Free PMC article.
-
Global prevalence of macrolide-resistant Staphylococcus spp.: a comprehensive systematic review and meta-analysis.Front Microbiol. 2025 Mar 14;16:1524452. doi: 10.3389/fmicb.2025.1524452. eCollection 2025. Front Microbiol. 2025. PMID: 40182286 Free PMC article.
-
Global patterns of antibiotic resistance in group B Streptococcus: a systematic review and meta-analysis.Front Microbiol. 2025 Apr 16;16:1541524. doi: 10.3389/fmicb.2025.1541524. eCollection 2025. Front Microbiol. 2025. PMID: 40342597 Free PMC article.
-
The prevalence of clarithromycin-resistant Helicobacter pylori isolates: a systematic review and meta-analysis.PeerJ. 2023 Mar 30;11:e15121. doi: 10.7717/peerj.15121. eCollection 2023. PeerJ. 2023. PMID: 37016679 Free PMC article.
-
The magnitude of antibiotic resistance to Helicobacter pylori in Africa and identified mutations which confer resistance to antibiotics: systematic review and meta-analysis.BMC Infect Dis. 2018 Apr 24;18(1):193. doi: 10.1186/s12879-018-3099-4. BMC Infect Dis. 2018. PMID: 29699490 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources

