Ocular ischemic syndrome secondary to cerebral aneurysms
- PMID: 39553911
- PMCID: PMC11566319
- DOI: 10.1016/j.ajoc.2024.102214
Ocular ischemic syndrome secondary to cerebral aneurysms
Abstract
Purpose: To describe the clinical findings in an 11-year-old male with a history of hemifacial microsomia presenting with ocular ischemic syndrome secondary to large cerebral aneurysms.
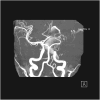
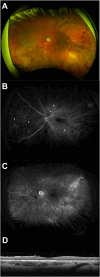
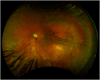
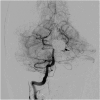
Observations: An 11-year-old male with a history of hemifacial microsomia presented to the Bascom Palmer Eye Institute Emergency Department complaining of nausea, diarrhea, headache, and decreased vision in the left eye. Visual acuity was light perception in the left eye and intraocular pressure was within normal limits. Gonioscopy revealed the presence of diffuse neovascularization of the angle. Posterior segment examination revealed mild vitreous hemorrhage, optic disc pallor, preretinal hemorrhage, generalized arteriolar narrowing, retinal microaneurysms, and abnormal arteriovenous communications with branching retinal vessels. Fluorescein angiography demonstrated patchy and delayed choroidal filling, a prolonged venous filling time, arteriolar attenuation, and vascular staining consistent with ocular ischemic syndrome. Magnetic resonance angiography was obtained which revealed large left internal carotid and anterior cerebral artery aneurysms. The patient underwent successful cerebral revascularization via bypass, ligation, clipping, and coiling procedures. At postoperative year 1, there was no evidence of ocular neovascularization and visual acuity remained light perception.
Conclusion and importance: Ocular ischemic syndrome is uncommon in children but may occur with any cause of ocular hypoperfusion. Hemifacial microsomia is a rare congenital disorder of craniofacial development caused by a vascular event in utero affecting the first and second branchial arches. This case demonstrates a rare cause of ocular ischemic syndrome and illustrates the potential for the development of clinically significant vascular abnormalities in patients with disorders of craniofacial development.
Keywords: Cerebral aneurysm; Hemifacial microsomia; Neovascularization; Ocular ischemic syndrome.
© 2024 The Authors. Published by Elsevier Inc.
Conflict of interest statement
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: AMB is a consultant for Alcon, Allergan, Zeiss, Dutch Ophthalmic Research Center, Novartis, ProQR, and Oculus. The following authors have no financial disclosures: LJR, PS, NFSC, CM, RMS, JJM.
Figures
References
-
- Mendrinos E., Machinis T.G., Pournaras C.J. Ocular ischemic syndrome. Surv Ophthalmol. 2010;55:2–34. - PubMed
-
- Brown G.C., Magargal L.E. The ocular ischemic syndrome. Clinical, fluorescein angiographic and carotid angiographic features. Int Ophthalmol. 1988;11:239–251. - PubMed
-
- Dugan J.D., Jr., Green W.R. Ophthalmologic manifestations of carotid occlusive disease. Eye (Lond) 1991;5(Pt 2):226–238. - PubMed
-
- Mizener J.B., Podhajsky P., Hayreh S.S. Ocular ischemic syndrome. Ophthalmology. 1997;104:859–864. - PubMed
-
- Hamed L.M., Guy J.R., Moster M.L., Bosley T. Giant cell arteritis in the ocular ischemic syndrome. Am J Ophthalmol. 1992;113:702–705. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

