Incidence of Postoperative Complications among Patients with Active or Resolved COVID-19 Undergoing Elective Abdominal Wall Reconstruction
- PMID: 39559265
- PMCID: PMC11573325
- DOI: 10.1097/GOX.0000000000006301
Incidence of Postoperative Complications among Patients with Active or Resolved COVID-19 Undergoing Elective Abdominal Wall Reconstruction
Abstract
Background: The incidence of postoperative complications among patients with coronavirus disease 2019 (COVID-19) positivity undergoing elective surgical operations is poorly understood. This study aimed to identify differences in postoperative complications after elective abdominal wall reconstruction (AWR) in patients diagnosed with COVID-19 compared with patients presenting prepandemic.
Methods: A single-institution, retrospective chart review was performed of patients undergoing AWR between January 2017 and September 2022. Patients were stratified by date: pre-COVID-19 (January 2017 to December 2019) and post-COVID-19 (January 2020 to September 2022). Patients confirmed as COVID-19-positive were also identified. Data collected included demographics, clinical characteristics, and complications. Univariate and multivariate analyses were performed.
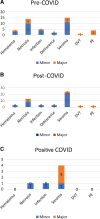
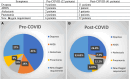
Results: We included 168 patients. The mean age was 54 years, and the mean body mass index was 33 kg/m2. Seventy-five patients underwent surgery pre-COVID-19 and 93 patients after. Of 93 patients, 16 (17%) had a positive COVID-19 test before surgery or during the perioperative period. These 2 groups were risk-matched. Patients with COVID-19 had no significant increase in postoperative complications. Major complications occurred at 13.3% in the pre-COVID-19 group and 7.5% in the post-COVID-19 group. Patients with COVID-19 were more likely to be younger (48 versus 57; P = 0.049) and more likely to have a shorter length of stay in the hospital (3 versus 5.8; P = 0.038).
Conclusions: In our case series, there was an associated increase in the incidence of overall pulmonary-related complications in the postpandemic group. This study is limited by its small sample size. Further investigation should be carried out on this topic.
Copyright © 2024 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of The American Society of Plastic Surgeons.
Conflict of interest statement
The authors have no financial interest to declare in relation to the content of this article.
Figures
References
-
- John Hopkins University. Coronavirus resource center. Available at https://coronavirus.jhu.edu/map.html. Published January 22, 2020. Accessed June 19, 2023.
-
- Jonker PKC, van der Plas WY, Steinkamp PJ, et al. ; Dutch Surgical COVID-19 Research Collaborative. Perioperative SARS-CoV-2 infections increase mortality, pulmonary complications, and thromboembolic events: a Dutch, multicenter, matched cohort clinical study. Surgery. 2021;169:264–274. - PMC - PubMed
LinkOut - more resources
Full Text Sources