Increased risk of migraine among patients with hidradenitis suppurativa: A US multi-center cohort study
- PMID: 39566658
- PMCID: PMC12166723
- DOI: 10.1016/j.bj.2024.100816
Increased risk of migraine among patients with hidradenitis suppurativa: A US multi-center cohort study
Abstract
Background: Hidradenitis suppurativa (HS) and migraine share common inflammatory pathways and neuropsychological implications. Both conditions involve proinflammatory cytokines like tumor necrosis factor and are associated with psychological comorbidities. Despite these similarities, the association between HS and migraine remained unclear. This study aimed to evaluate the relation between HS and incident migraine.
Materials and methods: We conducted a multicenter cohort study using the TriNetX Research Network. Patients diagnosed with HS between January 1, 2005, and December 31, 2022, were identified with a control group of non-HS subjects established by propensity score matching at a 1:1 ratio. Our outcome was the hazard ratio (HR) of incident migraine in relation to HS. We also examined the HR for various subtypes of migraine. We conducted stratified analyses based on age, gender, insomnia, depression, and anxiety subgroups. Sensitivity analyses were performed to strengthen the robustness of our analysis.
Results: The HS group exhibited an increased risk of incident migraine compared to controls (HR 1.35, 95% confidence interval (CI) 1.28-1.42). Also, HS patients had increased risk of migraine with aura and migraine without aura than controls, with HR being 1.36 (95% CI 1.21-1.52), 1.31 (95% CI 1.20-1.45), respectively. Female HS patients demonstrated an increased risk of incident migraine compared to their controls (HR 1.38, 95% CI 1.30-1.45). Elevated risk of incident migraine was observed in both younger and older HS patients when compared to their respective controls. The increased risk of incident migraine among HS patients remained consistent across various sensitivity analyses.
Conclusions: HS patients present with an increased risk of incident migraine. Physicians should be aware of this association and provide timely referrals and interventions when appropriate.
Keywords: Cohort studies; Electronic medical records; Hidradenitis suppurativa; TriNetX; migraine.
Copyright © 2024 The Authors. Published by Elsevier B.V. All rights reserved.
Conflict of interest statement
Conflicts of interest None.
Figures
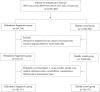

References
-
- Sabat R, Jemec GB, Matusiak Ł, Kimball AB, Prens E, Wolk K. Hidradenitis suppurativa. Nat Rev Dis Prim. 2020;6(1):18. - PubMed
-
- Kadylak D, Baranska-Rybak W. Botulinum toxin type A therapy for hidradenitis suppurativa: a case series. Dermatol Sin. 2023;41(2):121–122.
-
- Lewandowski M, Swierczewska Z, Baranska-Rybak W. YouTube as a source of information for hidradenitis suppurativa treatment. Dermatol Sin. 2022;40(3):156–161.
-
- Kluger N, Nuutinen P, Lybeck E, Ruohoalho TT, Salava A. Migraine is not the most common comorbidity in hidradenitis suppurativa patients. J Eur Acad Dermatol Venereol. 2019;33(9):e330–1. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

