Diagnostic performance of artificial intelligence in detecting oral potentially malignant disorders and oral cancer using medical diagnostic imaging: a systematic review and meta-analysis
- PMID: 39568787
- PMCID: PMC11576460
- DOI: 10.3389/froh.2024.1494867
Diagnostic performance of artificial intelligence in detecting oral potentially malignant disorders and oral cancer using medical diagnostic imaging: a systematic review and meta-analysis
Abstract
Objective: Oral cancer is a widespread global health problem characterised by high mortality rates, wherein early detection is critical for better survival outcomes and quality of life. While visual examination is the primary method for detecting oral cancer, it may not be practical in remote areas. AI algorithms have shown some promise in detecting cancer from medical images, but their effectiveness in oral cancer detection remains Naïve. This systematic review aims to provide an extensive assessment of the existing evidence about the diagnostic accuracy of AI-driven approaches for detecting oral potentially malignant disorders (OPMDs) and oral cancer using medical diagnostic imaging.
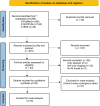
Methods: Adhering to PRISMA guidelines, the review scrutinised literature from PubMed, Scopus, and IEEE databases, with a specific focus on evaluating the performance of AI architectures across diverse imaging modalities for the detection of these conditions.
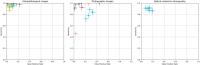
Results: The performance of AI models, measured by sensitivity and specificity, was assessed using a hierarchical summary receiver operating characteristic (SROC) curve, with heterogeneity quantified through I2 statistic. To account for inter-study variability, a random effects model was utilized. We screened 296 articles, included 55 studies for qualitative synthesis, and selected 18 studies for meta-analysis. Studies evaluating the diagnostic efficacy of AI-based methods reveal a high sensitivity of 0.87 and specificity of 0.81. The diagnostic odds ratio (DOR) of 131.63 indicates a high likelihood of accurate diagnosis of oral cancer and OPMDs. The SROC curve (AUC) of 0.9758 indicates the exceptional diagnostic performance of such models. The research showed that deep learning (DL) architectures, especially CNNs (convolutional neural networks), were the best at finding OPMDs and oral cancer. Histopathological images exhibited the greatest sensitivity and specificity in these detections.
Conclusion: These findings suggest that AI algorithms have the potential to function as reliable tools for the early diagnosis of OPMDs and oral cancer, offering significant advantages, particularly in resource-constrained settings.
Systematic review registration: https://www.crd.york.ac.uk/, PROSPERO (CRD42023476706).
Keywords: AI algorithms; OPMDs; deep learning; diagnostic performance; early detection; medical diagnostic imaging; oral cancer.
© 2024 Sahoo, Sahoo, Dash, Kumar, Baliarsingh, Panda and Pati.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

Similar articles
-
Application of artificial intelligence in the diagnosis of subepithelial lesions using endoscopic ultrasonography: a systematic review and meta-analysis.Front Oncol. 2022 Aug 15;12:915481. doi: 10.3389/fonc.2022.915481. eCollection 2022. Front Oncol. 2022. PMID: 36046054 Free PMC article.
-
Diagnostic Accuracy of Artificial Intelligence Compared to Biopsy in Detecting Early Oral Squamous Cell Carcinoma: A Systematic Review and Meta Analysis.Asian Pac J Cancer Prev. 2024 Aug 1;25(8):2593-2603. doi: 10.31557/APJCP.2024.25.8.2593. Asian Pac J Cancer Prev. 2024. PMID: 39205556 Free PMC article.
-
Diagnostic Accuracy of Artificial Intelligence Based on Imaging Data for Preoperative Prediction of Microvascular Invasion in Hepatocellular Carcinoma: A Systematic Review and Meta-Analysis.Front Oncol. 2022 Feb 24;12:763842. doi: 10.3389/fonc.2022.763842. eCollection 2022. Front Oncol. 2022. PMID: 35280776 Free PMC article.
-
Convolutional neural network-based artificial intelligence for the diagnosis of early esophageal cancer based on endoscopic images: A meta-analysis.Saudi J Gastroenterol. 2022 Sep-Oct;28(5):332-340. doi: 10.4103/sjg.sjg_178_22. Saudi J Gastroenterol. 2022. PMID: 35848703 Free PMC article. Review.
-
Diagnostic accuracy of artificial intelligence for detecting gastrointestinal luminal pathologies: A systematic review and meta-analysis.Front Med (Lausanne). 2022 Nov 4;9:1018937. doi: 10.3389/fmed.2022.1018937. eCollection 2022. Front Med (Lausanne). 2022. PMID: 36405592 Free PMC article.
Cited by
-
Knowledge level of diagnostic procedures and risk factors for oral cancer among oral healthcare providers in Germany.BMC Oral Health. 2025 May 2;25(1):681. doi: 10.1186/s12903-025-06048-5. BMC Oral Health. 2025. PMID: 40317003 Free PMC article.
-
Artificial intelligence and the diagnosis of oral cavity cancer and oral potentially malignant disorders from clinical photographs: a narrative review.Front Oral Health. 2025 Mar 10;6:1569567. doi: 10.3389/froh.2025.1569567. eCollection 2025. Front Oral Health. 2025. PMID: 40130020 Free PMC article. Review.
-
Evaluation of deepseek, gemini, ChatGPT-4o, and perplexity in responding to salivary gland cancer.BMC Oral Health. 2025 Aug 23;25(1):1358. doi: 10.1186/s12903-025-06726-4. BMC Oral Health. 2025. PMID: 40849657 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources

