Incidence and characterization of secondary CNS lymphoma in 1972 patients with DLBCL: a Danish nationwide cohort study
- PMID: 39571170
- PMCID: PMC11876834
- DOI: 10.1182/bloodadvances.2024014404
Incidence and characterization of secondary CNS lymphoma in 1972 patients with DLBCL: a Danish nationwide cohort study
Abstract
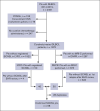
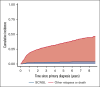
Secondary central nervous system lymphoma (SCNSL) is a rare manifestation of diffuse large B-cell lymphoma (DLBCL) with a poor prognosis. We present updated data from a nationwide study on the incidence and clinical characteristics of SCNSL. The incidence of SCNSL was calculated considering death or relapse without SCNSL as competing risks. Risk factors associated with SCNSL were identified using a cause-specific Cox proportional hazards model. A total of 1972 patients with DLBCL were included, of which 68 (3.4%) experienced SCNSL at the first relapse. The crude 1- and 2-year cumulative incidence of SCNSL was 2.0% (95% confidence interval [CI], 1.5-2.7) and 2.6% (95% CI, 2.0-3.4), respectively. For patients with a high-risk central nervous system international prognostic index (CNS-IPI) score, the 1- and 2-year cumulative incidence was 6.4% and 7.5%, respectively. The number and location of extranodal (EN) sites were the most significant predictors of SCNSL. Specific EN sites associated with an increased risk were the bone marrow, heart, kidneys/adrenal glands, ovaries, testes, and uterus. The median overall survival (OS) after SCNSL was 3.2 months. SCNSL within 6 months after the end of treatment (EOT) was associated with a higher baseline CNS-IPI score and worse OS than SCNSL >6 months after EOT. Patients with a combination of low-risk CNS-IPI and late-onset SCNSL had the most favorable prognosis. In conclusion, updated real-world population-based data on SCNSL at first relapse, adjusted for competing risks, demonstrated a lower incidence of SCNSL than previously reported, with the number and location of EN sites being the most significant predictors of SCNSL.
© 2025 American Society of Hematology. Published by Elsevier Inc. Licensed under Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0), permitting only noncommercial, nonderivative use with attribution. All other rights reserved.
Conflict of interest statement
Conflict-of-interest disclosure: M.R.C. reports consultancy for AbbVie, AstraZeneca, Genmab, Gilead, Incyte, Janssen, and Roche, and has received funding for travel expenses from AbbVie, AstraZeneca, Genmab, Janssen, Pfizer, and Roche. A.L.A.-M. has received funding from Genentech Inc. C.B. has received honoraria from Octapharma and AstraZeneca. C.U.N. has received research grants and/or consultancy fees from AbbVie, AstraZeneca, Janssen, Lilly, Genmab, BeiGene, Octapharma, CSL Behring, MSD, and Takeda. L.M.P. received a research grant from AbbVie. The remaining authors declare no competing financial interests.
Figures



References
-
- Coiffier B, Thieblemont C, Van Den Neste E, et al. Long-term outcome of patients in the LNH-98.5 trial, the first randomized study comparing rituximab-CHOP to standard CHOP chemotherapy in DLBCL patients: a study by the Groupe d’Etudes des Lymphomes de l’Adulte. Blood. 2010;116(12):2040–2045. - PMC - PubMed
-
- Schmitz N, Zeynalova S, Nickelsen M, et al. CNS International Prognostic Index: a risk model for CNS relapse in patients with diffuse large B-cell lymphoma treated with R-CHOP. J Clin Oncol. 2016;34(26):3150–3156. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

