The volume-outcome relationship for pulmonary endarterectomy in chronic thromboembolic pulmonary hypertension
- PMID: 39572220
- PMCID: PMC11865742
- DOI: 10.1183/13993003.01865-2024
The volume-outcome relationship for pulmonary endarterectomy in chronic thromboembolic pulmonary hypertension
Abstract
Background: We conducted a volume-outcome meta-analysis of pulmonary endarterectomy procedures for chronic thromboembolic pulmonary hypertension to objectively determine the minimum required annual case load that can define a high-volume centre.
Methods: Three electronic databases were systematically queried up to 1 May 2024. Centres were divided in volume tertiles. The primary outcomes were early mortality and long-term survival. Restricted cubic splines were used to demonstrate the volume-outcome relationship and the elbow-method was applied to define high-volume centres. Long-term survival was assessed using Cox frailty models.
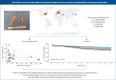
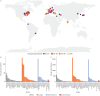
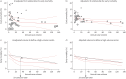
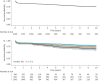
Results: We included 51 centres (52 consecutive cohorts) and divided them into tertiles (T1: <6 cases per year; T2: 6-15 cases per year, T3: >15 cases per year), comprising a total 11 345 patients (mean age 52.3 years). Overall early mortality was 6.0% (T1: 11.6%; T2: 7.2%; T3: 5.2%; p<0.001), for which a significant nonlinear volume-outcome relationship was observed (p=0.0437) with a statistically determined minimal required volume of 33 cases per year (95% CI 29-35 cases), and a modelled volume of 40 cases per year corresponding to a 5.0% mortality rate. Nevertheless, early mortality still progressively declined in higher volume centres (from 6.7% to 5.4% to 2.9% in centres performing 16-50, 51-100 and >100 procedures annually). In addition, a significant volume effect was observed for long-term survival (adjusted hazard ratio per tertile 0.75, 95% CI 0.63-0.89; p=0.001).
Conclusion: There is a significant association between procedural volume and early mortality in pulmonary endarterectomy. An annual procedural volume of >33-40 cases per year may be used to define a high‑volume centre, although higher volumes still lead to progressively lower mortality rates.
Copyright ©The authors 2025.
Conflict of interest statement
Conflict of interest: The authors have no potential conflicts of interest to disclose.
Figures
Comment in
-
Caseload in pulmonary endarterectomy: what defines expertise?Eur Respir J. 2025 Feb 27;65(2):2402399. doi: 10.1183/13993003.02399-2024. Print 2025 Feb. Eur Respir J. 2025. PMID: 40015736 No abstract available.
References
-
- Durrington C, Hurdman JA, Elliot CA, et al. Systematic pulmonary embolism follow-up increases diagnostic rates of chronic thromboembolic pulmonary hypertension and identifies less severe disease: results from the ASPIRE Registry. Eur Respir J 2024; 63: 2300846. doi: 10.1183/13993003.00846-2023 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
