Clinical features of anti-SAE1 antibody-positive myositis and interstitial lung disease: a multicenter, retrospective study in Taiwan
- PMID: 39575249
- PMCID: PMC11579618
- DOI: 10.3389/fimmu.2024.1482000
Clinical features of anti-SAE1 antibody-positive myositis and interstitial lung disease: a multicenter, retrospective study in Taiwan
Abstract
Introduction: The clinical characteristics of patients positive for anti-small ubiquitin-like modifier 1-activating enzyme subunit 1 (SAE1) antibodies and diagnosed with idiopathic inflammatory myopathies (IIMs) vary across different cohorts and ethnicities, particularly concerning interstitial lung disease (ILD). We aimed to assess the clinical utility of the line immunoblot assay (LIA) in detecting anti-SAE1 autoantibodies and evaluate the clinical relevance and chronology of ILD development in relation to SAE1 autoantibody positivity among Taiwanese patients.
Methods: We retrospectively conducted a population-based cohort analysis involving 6,496 patients who visited Chang Gung Memorial Health System across Taiwan from May 2018 to December 2021. Patients were assayed for myositis-specific autoantibodies (MSAs) and myositis-associated autoantibodies (MAAs) using the LIA method, and the antinuclear antibody (ANA) indirect immunofluorescence (IIF) method was used to evaluate ANA patterns. Of these, 70 SAE1-positive patients (1.08%) were included and followed up until December 2023. Associations with clinical characteristics and final diagnosis, particularly ILD, were assessed.
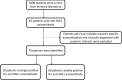
Results: Among the 70 SAE1-positive patients, 10 (14.3%) were strongly positive and 60 (85.7%) were weakly positive. In the strong positive group, 70% (7/10) were diagnosed with IIM, with most (5/7) showing a concordant ANA IIF pattern (speckled type). Six patients presented ILD either before (1/6) or after (5/6) IIM diagnosis; the majority (4/6) were classified as organizing pneumonia. The remaining 30.0% (3/10) had connective tissue disease (CTD) other than IIM without detectable ILD during follow-up, and none demonstrated a concordant ANA IIF pattern. In the weakly positive group, only 5.0% (3/60) had IIM and 3.3% (2/60) had ILD. The positive predictive value for strong positive SAE1 autoantibodies in diagnosing IIM was significantly higher than for weak positives (70.0% vs. 5.0%; p < 0.001).
Conclusions: The study suggests that strong positive SAE1 autoantibodies detected via LIA are more closely associated with IIM compared to weak positive results. A high prevalence of ILD was observed among strong positive Taiwanese patients, indicating the need for prompt screening. Patients with weak positive or discordant ANA IIF results may represent false positives with a lower ILD risk.
Keywords: anti-SAE1; autoantibody; autoimmune; idiopathic inflammatory myopathies; interstitial lung disease; positive predictive value.
Copyright © 2024 Hsiao, Tseng, Hsu, Chiu, Su and Chan.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Similar articles
-
Diagnosis of myositis-associated interstitial lung disease: Utility of the myositis autoantibody line immunoassay.Respir Med. 2021 Oct;187:106581. doi: 10.1016/j.rmed.2021.106581. Epub 2021 Aug 21. Respir Med. 2021. PMID: 34454312
-
Association of anti-Ro-52 antibodies with occurrence of interstitial lung disease in patients with idiopathic inflammatory myopathy.Arthritis Res Ther. 2024 Aug 22;26(1):152. doi: 10.1186/s13075-024-03382-x. Arthritis Res Ther. 2024. PMID: 39175076 Free PMC article.
-
[Clinical value of myositis antibodies in patients with connective tissue disease-associated interstitial lung diseases].Zhonghua Jie He He Hu Xi Za Zhi. 2019 Oct 12;42(10):765-770. doi: 10.3760/cma.j.issn.1001-0939.2019.10.010. Zhonghua Jie He He Hu Xi Za Zhi. 2019. PMID: 31594111 Chinese.
-
Idiopathic inflammatory myopathies and the lung.Eur Respir Rev. 2015 Jun;24(136):216-38. doi: 10.1183/16000617.00002015. Eur Respir Rev. 2015. PMID: 26028634 Free PMC article. Review.
-
Myositis Antibodies and Interstitial Lung Disease.J Appl Lab Med. 2022 Jan 5;7(1):240-258. doi: 10.1093/jalm/jfab108. J Appl Lab Med. 2022. PMID: 34996093 Review.
References
-
- Lundberg IE, Tjärnlund A, Bottai M, Werth VP, Pilkington C, de Visser M, et al. . 2017 European League Against Rheumatism/American College of Rheumatology classification criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Ann Rheum Dis. (2017) 76:1955–64. doi: 10.1136/annrheumdis-2017-211468 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical