Comparison of efficacy and safety of etomidate with other anesthesia induction drugs for patients undergoing cardiac surgery: A systematic review and meta-analysis of randomized controlled trials
- PMID: 39584115
- PMCID: PMC11585772
- DOI: 10.1016/j.heliyon.2024.e38274
Comparison of efficacy and safety of etomidate with other anesthesia induction drugs for patients undergoing cardiac surgery: A systematic review and meta-analysis of randomized controlled trials
Abstract
Introduction: Etomidate is commonly used to induce anesthesia in cardiac surgery patients due to its favorable cardiovascular profile. Sedative-hypnotic effects are mediated by gammaaminobutyric acid (GABA) receptor complexes in the central nervous system. There are numerous studies in which etomidate and other drugs are compared in terms of their clinical outcomes. The relative efficacy and safety of etomidate, however, remains inconclusive. In this study, we performed a systematic analysis of randomized controlled trials to assess the impact of etomidate, on patients undergoing cardiac surgery, with respect to patient outcome and adverse events.
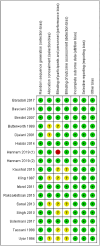
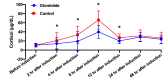
Methods: A systematic review was conducted of all existing clinical trials exploring the safety and efficacy of etomidate in patients undergoing cardiac surgery. Randomized controlled trials (RCTs) that compared etomidate with other drugs during induction in adult cardiac surgery assessing hemodynamic parameters and clinical outcomes were included, while studies involving non-cardiac or pediatric surgery and those lacking relevant outcome data were excluded. Primary outcomes were all-cause 30-day mortality. Secondary outcomes included duration of tracheal intubation, duration of intensive care unit (ICU) stay, duration of hospital stay, systolic blood pressure (SBP), diastolic blood pressure (DBP), mean arterial pressure (MAP), heart rate (HR) and other hemodynamic parameters, vasopressor requirements after induction and intubation, cortisol levels, and incidence of myoclonus.
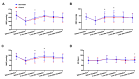
Results: Sixteen randomized controlled trials involving 1162 patients were included. Etomidate did not affect the all-cause 30-day mortality of patients undergoing cardiac surgery compared to comparator drugs (RR, 0.96; 95 % CI, 0.26 to 3.49; P = 0.95). There were no significant differences in the duration of tracheal intubation (MD, -0.08 h; 95 % CI, -1.96 to 1.81; P = 0.94), the duration of ICU stay (MD, -2.07 h; 95 % CI, -8.09 to 3.96; P = 0.50) or the duration of hospital stay (MD, -0.62 d; 95 % CI, -2.25 to 1.00; P = 0.45) when etomidate was compared to comparator drugs. Patients receiving etomidate demonstrated a more stable hemodynamic profile after induction and intubation compared to those receiving comparator drugs. The requirement of a vasopressor after induction and intubation was significantly reduced with etomidate compared with those with comparator drugs (RR, 0.37; 95 % CI, 0.25 to 0.56; P < 0.00001).
Conclusions: This systematic meta-analysis found a significant heterogeneity among included studies. In addition, most studies focused only on the hemodynamic profile of etomidate. Thus, efficacy and safety of etomidate could not be answered within this context. Nevertheless, for patients undergoing cardiac surgery, etomidate seems to offer a minimal beneficial cardiovascular profile in comparison with other agents during induction and intubation. However, improved hemodynamics did not improve clinical outcomes as Etomidate did not affect mortality, duration of tracheal intubation, the length of stay in ICU and hospital. Finally, infectious side effects as one important trigger for increased mortality in ICU patients due to the use of Etomidate could not be analyzed as data were mostly missing.
© 2024 The Authors.
Conflict of interest statement
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests:Hanjun Wang reports financial support was provided by 10.13039/100000002National Institutes of Health. If there are other authors, they declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures






References
-
- Raksakietisak M., Ngamlamiad C., Duangrat T., Soontarinka S., Raksamani K. The changes in cortisol levels during cardiac surgery: a randomized double-blinded study between two induction agents etomidate and thiopentone. J. Med. Assoc. Thai. 2015;98:775–781. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

