Calculating Optimal Patient to Nursing Capacity: Comparative Analysis of Traditional and New Methods
- PMID: 39584562
- PMCID: PMC11612603
- DOI: 10.2196/59619
Calculating Optimal Patient to Nursing Capacity: Comparative Analysis of Traditional and New Methods
Abstract
Background: Optimal nurse staffing levels have been shown to impact patients' prognoses and safety, as well as staff burnout. The predominant method for calculating staffing levels has been patient-to-nurse (P/N) ratios and nursing hours per patient day. However, both methods fall short of addressing the dynamic nature of staffing needs that often fluctuate throughout the day as patients' clinical status changes and new patients are admitted or discharged from the unit.
Objective: In this evaluation, the Veterans Affairs Palo Alto Health Care System (VAPAHCS) piloted a new dynamic bed count calculation in an effort to target optimal staffing levels every hour to provide greater temporal resolution on nurse staffing levels within the Veterans Health Administration.
Methods: The dynamic bed count uses elements from both the nursing hours per patient day and P/N ratio to calculate current and target staffing levels, every hour, while balancing across nurse types (registered nurses to nurse assistants) to provide improved temporal insight into staff allocation. The dynamic bed count was compared with traditional P/N ratio methods of calculating patient capacity at the VAPAHCS, to assess optimal patient capacity within their acute care ward from January 1, 2023, through May 25, 2023. Descriptive statistics summarized patient capacity variables across the intensive care unit (ICU), medical-surgical ICU, and 3 acute care units. Student t tests (2-tailed) were used to analyze differences between patient capacity measures.
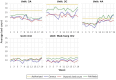
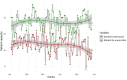
Results: Hourly analysis of patient capacity information displayed how the dynamic bed count provided improved temporal resolution on patient capacity. Comparing the dynamic bed count to the P/N ratio, we found the patient capacity, as determined by the P/N ratio, was, on average, higher than that of the dynamic bed count across VAPAHCS acute care units and the medical-surgical ICU (P<.001). For example, in acute care unit 3C, the average dynamic bed count was 21.6 (SD 4.2) compared with a P/N ratio of 28.6 (SD 3.2). This suggests that calculating patient capacity using P/N ratios alone could lead to units taking on more patients than what the dynamic bed count suggests the unit can optimally handle.
Conclusions: As a new patient capacity calculation, the dynamic bed count provided additional details and timely information about clinical staffing levels, patient acuity, and patient turnover. Implementing this calculation into the management process has the potential to empower departments to further optimize staffing and patient care.
Keywords: NHPPD; comparative analysis; nurse; nurse assistants; nurse scheduling; nurse staffing; nursing; nursing administration; nursing hours per patient day; patient capacity; patient ratio; registered nurses; staff allocation; staffing; workload.
© Anna Ware, Terri Blumke, Peter Hoover, David Arreola. Originally published in JMIR Nursing (https://nursing.jmir.org).
Conflict of interest statement
Figures
Similar articles
-
Nurse staffing and patient mortality in intensive care units.Nurs Res. 2008 Sep-Oct;57(5):322-30. doi: 10.1097/01.NNR.0000313498.17777.71. Nurs Res. 2008. PMID: 18794716
-
Estimating the Relationship Between Nurse Staffing and Medication Pass Workload Using National Barcode Data.Nurs Res. 2024 Nov-Dec 01;73(6):450-457. doi: 10.1097/NNR.0000000000000764. Epub 2024 Jul 17. Nurs Res. 2024. PMID: 39103311
-
The relationship between nurse staffing and patient outcomes.J Nurs Adm. 2003 Sep;33(9):478-85. doi: 10.1097/00005110-200309000-00008. J Nurs Adm. 2003. PMID: 14501564
-
A review of workload measures: a context for a new staffing methodology in Western Australia.Int J Nurs Stud. 2009 Jan;46(1):131-9. doi: 10.1016/j.ijnurstu.2008.08.005. Epub 2008 Sep 11. Int J Nurs Stud. 2009. PMID: 18789439 Review.
-
Hospital nurse-staffing models and patient- and staff-related outcomes.Cochrane Database Syst Rev. 2019 Apr 23;4(4):CD007019. doi: 10.1002/14651858.CD007019.pub3. Cochrane Database Syst Rev. 2019. PMID: 31012954 Free PMC article.
Cited by
-
2024: A Year of Nursing Informatics Research in Review.JMIR Nurs. 2025 May 7;8:e74345. doi: 10.2196/74345. JMIR Nurs. 2025. PMID: 40334285 Free PMC article.
References
-
- Chen YC, Guo YLL, Chin WS, Cheng NY, Ho JJ, Shiao JSC. Patient-nurse ratio is related to nurses’ intention to leave their job through mediating factors of burnout and job dissatisfaction. Int J Environ Res Public Health. 2019 Nov 29;16(23):4801. doi: 10.3390/ijerph16234801. doi. Medline. - DOI - PMC - PubMed
-
- Phillips J, Malliaris A, Bakerjian D. Nursing and patient safety. Patient Safety Network. 2021. [31-08-2023]. https://psnet.ahrq.gov/primer/nursing-and-patient-safety URL. Accessed.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

