Sex discrepancies in cancer research: a systematic review of prospective and retrospective investigations in lung, melanoma, and colorectal cancers
- PMID: 39588064
- PMCID: PMC11586390
- DOI: 10.3389/fgwh.2024.1445139
Sex discrepancies in cancer research: a systematic review of prospective and retrospective investigations in lung, melanoma, and colorectal cancers
Abstract
Introduction: According to the latest Cancer Statistics, colorectal, lung, and melanoma are three of the most common cancers that affect both males and females. While males have consistently had a higher incidence and mortality rate in all three types of cancers, females have been shown to have better outcomes. Sex discrepancies in cancer research can impact the efficacy and effectiveness of novel drugs and diagnostic tools. Study results may not accurately represent how the treatment or diagnostic tool performs in the underrepresented sex. To comprehensively assess sex representation in top non-sex-specific cancer research, this systematic review aims to identify if there is equal representation of males and females in colorectal, lung, and melanoma cancer research.
Methods: We explored retrospective and prospective clinical studies published in Pubmed from 2014 to 2023 to identify possible sex discrepancies in colorectal, lung, and melanoma cancer. MeSH terms were employed to retrieve relevant studies for each cancer type (colorectal, lung, melanoma). MeSH terms used include "lung cancer", "melanoma", and "colorectal cancer", in combination with "trials", "retrospective", and "prospective". Extracted data included study characteristics (author, year of publication), study design (prospective or retrospective), sample size, and the number of male and female participants.
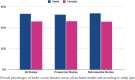
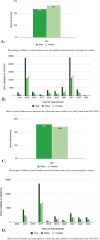
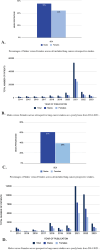
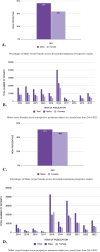
Results: The complete study population consisted of 515,003 patients, of which 275,231 (53%) were males and 237,488 (46%) were females. Specifically, retrospective studies included a total of 302,974 patients with 163,473 (54%) of them identifying as male and 139,072 (46%) patients identifying as female. While prospective studies included a total of 212,029 patients with 111,758 (53%) of these being male and 98,416 (46%) being female. Overall, male representation in the studies included in this systematic review was higher than female representation.
Discussion: Disparities in representation were identified in colorectal cancer, lung cancer, and melanoma cancer studies underscoring the need for equitable inclusion of both sexes in cancer research to advance precision medicine and improve patient outcomes. Further exploration of the impact of sex, race, and socioeconomic status on study representation is warranted.
Keywords: cancer research; colorectal cancer; health disparities; lung cancer; melanoma; prospective; retrospective; sex differences.
© 2024 Díaz Rosario, Vélez-Morell and Martinez.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- American Cancer Society. Understanding Cancer Research Study Design and how to Evaluate Results. Hoboken, NJ: American Cancer Society; (2013). Available online at: https://www.cancer.net/research-and-advocacy/introduction-cancer-researc... (cited March 13, 2024).
-
- SEER. Cancer Disparities - Cancer Stat Facts. Atlanta: NIH- National Cancer Institute. (2022). Available online at: https://seer.cancer.gov/statfacts/html/.html (cited March 13, 2024).
Publication types
LinkOut - more resources
Full Text Sources

