Perifoveal Exudative Vascular Anomalous Complex (PEVAC): Retinal Vascular Density Findings
- PMID: 39598024
- PMCID: PMC11595356
- DOI: 10.3390/jcm13226879
Perifoveal Exudative Vascular Anomalous Complex (PEVAC): Retinal Vascular Density Findings
Abstract
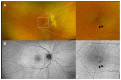
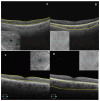
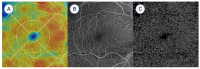
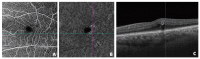
Objectives: This study aimed to describe the clinical, optical coherence tomography (OCT) and OCT angiography (OCTA) findings and characteristics in patients with perifoveal exudative vascular anomalous complex (PEVAC) and compare the macular vascular density with the age-matched control group. Methods: We conducted a case-control study to compare demographic information, clinical observations, and OCT/OCTA findings in eyes with PEVAC (n = 5 eyes in 5 patients) and a control group of subjects matched for age (n = 9). The Advanced Retina Imaging (ARI) network algorithms were utilized to evaluate OCTA observations. Statistical analysis was performed by the nonparametric Mann-Whitney U test. Results: Patients with PEVAC had a mean (±SD) age at presentation of 70 ± 12.6 years, the mean follow-up period was 7.8 ± 5.2 months, and unilateral disease was observed. Four out of the five patients in our cohort had a history of systemically treated hypertension and dyslipidemia. Three eyes had lesions in the inner temporal retinal zone, while the remaining two eyes had lesions in the inner inferior or central zone. Retina slab analysis using OCTA showed no significant difference in vascular density parameters between the PEVAC and control groups. Conclusions: Although limited by a small sample size, our study suggests that macular vessel density shows no significant difference between PEVAC cases and control eyes.
Keywords: ARI network; OCTA; PEVAC; vessel density.
Conflict of interest statement
Author Deborah Cosette was employed by the Carl Zeiss Meditec, Inc. No affiliated company was involved in the study design, data collection, analysis, or interpretation, manuscript writing, or the decision to publish the results.The remaining authors declare no conflicts of interest.
Figures
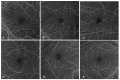
References
LinkOut - more resources
Full Text Sources

