Two-Year Outcomes Using Fast-Acting, Sub-Perception Therapy for Spinal Cord Stimulation: A European, Real-World, Multicenter Experience
- PMID: 39598142
- PMCID: PMC11595255
- DOI: 10.3390/jcm13226999
Two-Year Outcomes Using Fast-Acting, Sub-Perception Therapy for Spinal Cord Stimulation: A European, Real-World, Multicenter Experience
Abstract
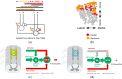
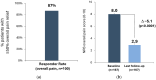
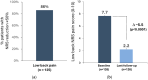
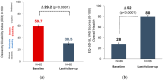
Background/Objectives: Over the last 20 years, spinal cord stimulation (SCS) has seen the development of various paresthesia-free paradigms. Recently, a novel modality has emerged (Fast-Acting Sub-perception Therapy, FAST) that engages the surrounding inhibition mechanism of action. We evaluated long-term, real-world outcomes of preferential FAST-SCS use in patients with chronic pain. Methods: In this multi-center, observational, consecutive case series, medical chart data from chronic pain patients preferentially using FAST-SCS (no exclusions) were retrospectively reviewed. Results: Data from 167 patients in 13 European centers were analyzed; 74% of patients suffered from persistent spine pain syndrome type 2 and 87% presented with low back and/or leg pain. At the last follow-up (mean 1.6 years), the numerical rating scale (NRS) overall pain score decreased by 5.1 ± 2.5 points versus baseline, from 8.0 ± 1.2 to 2.9 ± 2.2 (n = 167, p < 0.0001). 87% of patients reported ≥50% pain relief, and 55% were "high responders" with overall NRS pain scores ≤2/10. At the last follow-up, functional disability improved significantly (the Oswestry Disability Index reduced by 29.2 ± 21.5 points, n = 65, p < 0.0001) and patients had a significant gain in quality of life (EQ-5D-5L visual analog scale increased by 52.0 ± 26.9 points, n = 86, p < 0.0001). Results at the 2-year follow-up showed a sustained, substantial reduction in pain; 67% of patients were high responders and the NRS overall pain score decreased by 5.6 ± 2.4 versus baseline (n = 52, p < 0.0001). Conclusions: Our real-world outcomes suggest that in patients with chronic low back and/or leg pain, FAST-SCS therapy provided durable and profound pain relief and led to significant improvements in disability and quality of life.
Keywords: chronic pain; fast-acting; spinal cord stimulation; sub-perception; surround inhibition.
Conflict of interest statement
Simon Bayerl has received research grants from and occasionally works as a consultant and speaker for Boston Scientific. Georgios Matis has received honoraria from Abbott, Boston Scientific, Esteve Pharmaceuticals, Medtronic, Nevro, and Saluda Medical for presenting at symposia and serving as an instructor (cadaver labs, proctorships). Philippe Rigoard reports research grants and honoraria from Medtronic, Abbott, and Boston Scientific. Jan Willem Kallewaard has worked on advisory boards for Boston Scientific, Medtronic, and Saluda. Jan Vesper reports work as a consultant and on advisory boards, travel grants, and research grants from Boston Scientific. Ashish Gulve has attended a speaker panel and received honoraria from Medtronic, Boston, Nevro and Mainstay Medical. Sylvie Raoul has consulted for Boston Scientific, Abbot, and Medtronic. Sarah Love-Jones has worked on medical advisory boards for Boston Scientific, Medtronic, Nevro, Saluda, Pfizer, undertaken scientific research in collaboration with Boston Scientific, Mainstay Medical, Nalu Medical, Nevro, Saluda, and Abbott, and received honoraria for speaking at conferences from Boston Scientific, Nevro, and Saluda. Adam c has received honoraria from Boston Scientific and Saluda for speaking at symposia, participated on an advisory board for Saluda, and worked as a cadaveric instructor for Boston Scientific. Jose Paz-Solis, M. Angeles Canos-Verdecho, Georgios Kyriakopoulos, Jose Emilio Llopis, and Alfonso Papa declare no conflict of interest.
Figures


References
-
- Veizi E., Hayek S.M., North J., Chafin T.B., Yearwood T.L., Raso L., Frey R., Cairns K., Berg A., Brendel J., et al. Spinal Cord Stimulation (SCS) with Anatomically Guided (3D) Neural Targeting Shows Superior Chronic Axial Low Back Pain Relief Compared to Traditional SCS—LUMINA Study. Pain Med. 2017;18:1534–1548. doi: 10.1093/pm/pnw286. - DOI - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

