A Prediction Model to Identify Clinically Relevant Medication Discrepancies at the Emergency Department (MED-REC Predictor): Development and Validation Study
- PMID: 39602806
- PMCID: PMC11635314
- DOI: 10.2196/55185
A Prediction Model to Identify Clinically Relevant Medication Discrepancies at the Emergency Department (MED-REC Predictor): Development and Validation Study
Abstract
Background: Many patients do not receive a comprehensive medication reconciliation, mostly owing to limited resources. We hence need an approach to identify those patients at the emergency department (ED) who are at increased risk for clinically relevant discrepancies.
Objective: The aim of our study was to develop and externally validate a prediction model to identify patients at risk for at least 1 clinically relevant medication discrepancy upon ED presentation.
Methods: A prospective, multicenter, observational study was conducted at the University Hospitals Leuven and General Hospital Sint-Jan Brugge-Oostende AV, Belgium. Medication histories were obtained from patients admitted to the ED between November 2017 and May 2022, and clinically relevant medication discrepancies were identified. Three distinct datasets were created for model development, temporal external validation, and geographic external validation. Multivariable logistic regression with backward stepwise selection was used to select the final model. The presence of at least 1 clinically relevant discrepancy was the dependent variable. The model was evaluated by measuring calibration, discrimination, classification, and net benefit.
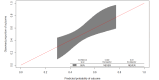
Results: We included 824, 350, and 119 patients in the development, temporal validation, and geographic validation dataset, respectively. The final model contained 8 predictors, for example, age, residence before admission, number of drugs, and number of drugs of certain drug classes based on Anatomical Therapeutic Chemical coding. Temporal validation showed excellent calibration with a slope of 1.09 and an intercept of 0.18. Discrimination was moderate with a c-index (concordance index) of 0.67 (95% CI 0.61-0.73). In the geographic validation dataset, the calibration slope and intercept were 1.35 and 0.83, respectively, and the c-index was 0.68 (95% CI 0.58-0.78). The model showed net benefit over a range of clinically reasonable threshold probabilities and outperformed other selection criteria.
Conclusions: Our software-implemented prediction model shows moderate performance, outperforming random or typical selection criteria for medication reconciliation. Depending on available resources, the probability threshold can be customized to increase either the specificity or the sensitivity of the model.
Keywords: MED-REC; MED-REC predictor; emergency department; geographic; geographic validation; hospital; medication; medication discrepancy; medication reconciliation; patient; prediction model; predictor; risk stratification; software; software-implemented prediction model.
©Greet Van De Sijpe, Matthias Gijsen, Lorenz Van der Linden, Stephanie Strouven, Eline Simons, Emily Martens, Nele Persan, Veerle Grootaert, Veerle Foulon, Minne Casteels, Sandra Verelst, Peter Vanbrabant, Sabrina De Winter, Isabel Spriet. Originally published in the Journal of Medical Internet Research (https://www.jmir.org), 27.11.2024.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures




References
-
- Pippins JR, Gandhi TK, Hamann C, Ndumele CD, Labonville SA, Diedrichsen EK, Carty MG, Karson AS, Bhan I, Coley CM, Liang CL, Turchin A, McCarthy PC, Schnipper JL. Classifying and predicting errors of inpatient medication reconciliation. J Gen Intern Med. 2008;23(9):1414–1422. doi: 10.1007/s11606-008-0687-9. https://europepmc.org/abstract/MED/18563493 - DOI - PMC - PubMed
-
- Tam VC, Knowles SR, Cornish PL, Fine N, Marchesano R, Etchells EE. Frequency, type and clinical importance of medication history errors at admission to hospital: a systematic review. CMAJ. 2005;173(5):510–515. doi: 10.1503/cmaj.045311. http://www.cmaj.ca/cgi/pmidlookup?view=long&pmid=16129874 173/5/510 - DOI - PMC - PubMed
-
- van Cauwenberghe L, van Kemseke S, Oudaert E, Pauwels S, Steurbaut S, van Laere S, Hubloue I. Interception of chronic medication discrepancies by the clinical pharmacist in the emergency department. Eur J Emerg Med. 2023;30(1):7–14. doi: 10.1097/MEJ.0000000000000961.00063110-202302000-00004 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

