Cardiovascular benefits and safety profile of macrolide maintenance therapy in patients with bronchiectasis
- PMID: 39603670
- PMCID: PMC11883147
- DOI: 10.1183/13993003.01574-2024
Cardiovascular benefits and safety profile of macrolide maintenance therapy in patients with bronchiectasis
Abstract
Background: Macrolide maintenance therapy (MMT) has demonstrated notable efficacy in reducing exacerbation in patients with bronchiectasis, which is a major risk factor for cardiovascular events. However, a comprehensive assessment of the cardiovascular benefits and safety profile of MMT in this population is lacking.
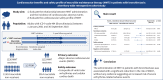
Methods: This territory-wide cohort study analysed patients diagnosed with bronchiectasis in Hong Kong between 2001 and 2018. Patients were classified as MMT receivers or macrolide non-receivers based on the administration of MMT. Propensity score (PS) matching was employed for confounding factors adjustment. The primary outcome of interest was major adverse cardiovascular events (MACE), a composite of cardiovascular death, myocardial infarction and stroke. The safety outcome was the occurrence of ventricular arrhythmias or sudden cardiac death. Cox proportional hazard regression analysis was utilised to compare the incidence of outcomes across the two groups.
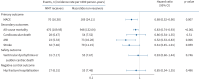
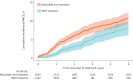
Results: A total of 22 895 patients with bronchiectasis were identified. Following 1:2 PS matching, the final cohort consisted of 3137 individuals, with 1123 MMT receivers and 2014 macrolide non-receivers. MMT administration was associated with a significantly reduced risk of MACE (16.38 versus 24.11 events per 1000 person-years; hazard ratio (HR) 0.68, 95% CI 0.52-0.90). Importantly, the use of MMT was not associated with elevated risk of ventricular arrhythmias or sudden cardiac death (7.17 versus 7.67 events per 1000 person-years; HR 0.93, 95% CI 0.60-1.44).
Conclusions: The administration of MMT in patients with bronchiectasis was associated with a significant reduction in the risk of MACE, without any evidence suggesting an increased risk of severe arrhythmia-related adverse events.
Copyright ©The authors 2025.
Conflict of interest statement
Conflict of interest: D. Wat has received speaker's fees from Chiesi, AstraZeneca, GSK, Sterling Anglian, Glenmark and Insmed. F. Frost has received speaker's fees from Chiesi, AstraZeneca and Vertex Pharmaceuticals, and support for attending meetings and travel from Chiesi. The research presented in this manuscript was conducted independently, and the authors declare that there was no impact of the conflicts of interest on the work. The remaining authors have no potential conflicts of interest to disclose.
Figures

Comment in
-
Unbreak my heart: macrolide cardiovascular benefits and safety in bronchiectasis.Eur Respir J. 2025 Mar 6;65(3):2500045. doi: 10.1183/13993003.00045-2025. Print 2025 Mar. Eur Respir J. 2025. PMID: 40049740 No abstract available.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
