Current Concepts and Medical Management for Patients with Radiographic Axial Spondyloarthritis
- PMID: 39620565
- PMCID: PMC11638751
- DOI: 10.5371/hp.2024.36.4.234
Current Concepts and Medical Management for Patients with Radiographic Axial Spondyloarthritis
Abstract
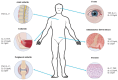
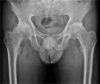
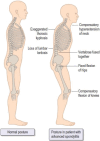
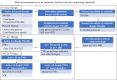
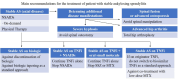
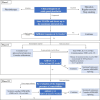
Radiographic axial spondyloarthritis (r-axSpA), a chronic inflammatory disease, can cause significant radiographic damage to the axial skeleton. Regarding the pathogenic mechanism, association of r-axSpA with tumor necrosis factor (TNF) and the interleukin-23/17 (IL23/ IL17) pathway has been reported. Development of extraarticular manifestations, including uveitis, inflammatory bowel disease, and psoriasis, has been reported in some patients. The pivotal role of human leukocyte antigen-B27 in the pathogenesis of r-axSpA remains to be clarified. Symptoms usually start in late adolescence or early adulthood, and disease progression can vary in each patient, with clinical manifestations ranging from mild joint stiffness without radiographic changes to advanced manifestations including complete fusion of the spine, and severe arthritis of the hip, and could include peripheral arthritis and extraarticular manifestations. The modified New York criteria was used previously in diagnosis of r-axSpA. However, early diagnosis of the disease prior to development of bone deformity was required due to development of biological agents. As a result of Assessment of SpondyloArthritis international Society (ASAS), the classification was improved in part for diagnosis of spondyloarthritis prior to development of bone deformity. The diagnosis is based on comprehensive laboratory findings, physical examinations, and radiologic findings. Medical treatment for r-axSpA involves the use of a stepwise strategy, starting with administration of nonsteroidal anti-inflammatory drugs and physiotherapy, and progressing to sulfasalazine or methotrexate and biologics including TNF-α inhibitors or IL-17 inhibitors as needed. Use of Janus kinase inhibitors has been recently reported.
Keywords: Ankylosing spondylitis; Axial spondyloarthritis.
Conflict of interest statement
Jeong Joon Yoo has been a Section Chief Editor since June 2021, but had no role in the decision to publish this article. No other potential conflict of interest relevant to this article was reported.
Figures
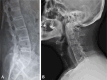
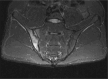
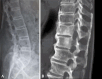
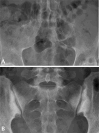
References
-
- Olivieri I, van Tubergen A, Salvarani C, van der Linden S. Seronegative spondyloarthritides. Best Pract Res Clin Rheumatol. 2002;16:723–39. doi: 10.1053/berh.2002.0263. https://doi.org/10.1053/berh.2002.0263. - DOI - PubMed
-
- Braun J, Sieper J. Ankylosing spondylitis. Lancet. 2007;369:1379–90. doi: 10.1016/S0140-6736(07)60635-7. https://doi.org/10.1016/s0140-6736(07)60635-7. - DOI - PubMed
-
- Khan MA. Ankylosing spondylitis: a dual perspective of current issues and challenges. J Rheumatol Suppl. 2006;78:1–3. - PubMed
-
- Zeng QY. Ankylosing spondylitis in Shantou, China: 15 years' clinical experience. J Rheumatol. 2003;30:1816–21. - PubMed
-
- Rudwaleit M, van der Heijde D, Landewé R, et al. The development of Assessment of SpondyloArthritis International Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis. 2009;68:777–83. doi: 10.1136/ard.2009.108233. https://doi.org/10.1136/ard.2009.108233. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials

