Effect of Acupoint Catgut Embedding on Subjective Appetite in Overweight and Obese Adults with Strong and Moderate Appetite: A Secondary Analysis of a Randomized Clinical Trial
- PMID: 39635504
- PMCID: PMC11614713
- DOI: 10.2147/DMSO.S487877
Effect of Acupoint Catgut Embedding on Subjective Appetite in Overweight and Obese Adults with Strong and Moderate Appetite: A Secondary Analysis of a Randomized Clinical Trial
Abstract
Background: Appetite plays a crucial role in obesity and weight loss outcomes. while conventional therapies reduce appetite, They often have limitations. Acupoint Catgut Embedding (ACE) is widely used for weight loss, but its impact on subjective appetite, especially across different appetite status, remains underexplored.
Objective: To evaluate the differential impact of ACE on the subjective appetite of overweight and obese adults with strong and moderate appetites.
Methods: This secondary analysis used data from a multicenter, double-blind, parallel randomized clinical trial of the ACE intervention. A total of 122 overweight and obese patients aged 18-60 were randomly assigned to the ACE and Non-acupoint Catgut Embedding (NACE) groups, each receiving six sessions over 12 weeks and a 4-week follow-up. Appetite was measured using the Visual Analogue Scale (VAS), and a generalized linear mixed-effects model assessed changes in appetite scores. Bonferroni corrections were applied for multiple comparisons (P < 0.05).
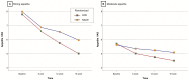
Results: Participants with strong appetite in the ACE group showed a significant reduction in appetite VAS score from 7.78 (0.66) at baseline to 5.00 (0.72) at 16 weeks (P < 0.05), compared to a reduction from 7.97 (0.93) to 6.54 (1.17) in the NACE group. The adjusted relative rate ratio between the two groups was 0.411 (95% CI, 0.210 to 0.534; P < 0.05). In participants with moderate appetite, no significant difference was observed between the two groups (P > 0.05). The significant baseline difference in appetite scores between participants with strong and moderate appetite (P < 0.05) became non-significant by week 16 (P > 0.05).
Conclusion: This study reveals the stratified effect of ACE on appetite, with greater reduction in those with strong appetite and no significant change in those with moderate appetite. This suggests ACE reduces appetite effectively without excessive suppression, supporting its potential as a sustainable obesity management strategy.
Keywords: acupoint catgut embedding; appetite; obesity; overweight; randomized controlled trial.
© 2024 Tang et al.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
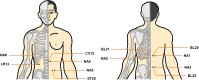
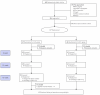
Figures

Similar articles
-
Effect of Acupoint Catgut Embedding for Abdominally Obese Female with Strong Appetite: Mixed Analysis of a Randomized Clinical Trial.Diabetes Metab Syndr Obes. 2022 Oct 31;15:3387-3395. doi: 10.2147/DMSO.S388485. eCollection 2022. Diabetes Metab Syndr Obes. 2022. PMID: 36341230 Free PMC article.
-
The Effect of Catgut Embedding at Acupoints Versus Nonacupoints in Abdominal Obesity: Protocol for a Multicenter, Double-Blind, 16-Week Randomized Controlled Trial.JMIR Res Protoc. 2023 Jul 10;12:e46863. doi: 10.2196/46863. JMIR Res Protoc. 2023. PMID: 37428535 Free PMC article.
-
Effect of catgut embedding at acupoints versus non-acupoints in abdominal obesity: a randomized clinical trial.J Tradit Chin Med. 2023 Aug;43(4):780-786. doi: 10.19852/j.cnki.jtcm.20230608.002. J Tradit Chin Med. 2023. PMID: 37454263 Free PMC article. Clinical Trial.
-
Comparing verum and sham acupoint catgut embedding for adults with obesity: A systematic review and meta-analysis of randomized clinical trials.Medicine (Baltimore). 2024 Jan 26;103(4):e36653. doi: 10.1097/MD.0000000000036653. Medicine (Baltimore). 2024. PMID: 38277544 Free PMC article.
-
[Clinical randomized controlled trials of acupoint catgut-embedding for simple obesity: a meta-analysis].Zhongguo Zhen Jiu. 2014 Jun;34(6):621-6. Zhongguo Zhen Jiu. 2014. PMID: 25112111 Review. Chinese.
Cited by
-
Application of Polyglycolic Acid/Poly (Lactic-co-glycolic Acid) in Thread Embedding Acupuncture for Obesity: New Strategies and Challenges.Diabetes Metab Syndr Obes. 2025 Jul 5;18:2175-2189. doi: 10.2147/DMSO.S525783. eCollection 2025. Diabetes Metab Syndr Obes. 2025. PMID: 40636750 Free PMC article. Review.
References
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

