Development and validation of a nomogram-based risk prediction model for carbapenem-resistant Klebsiella pneumoniae in hospitalized patients
- PMID: 39641574
- PMCID: PMC11705954
- DOI: 10.1128/spectrum.02170-24
Development and validation of a nomogram-based risk prediction model for carbapenem-resistant Klebsiella pneumoniae in hospitalized patients
Abstract
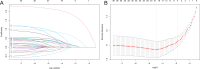
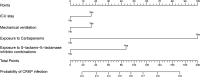
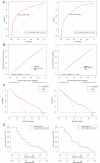
Carbapenem-resistant Klebsiella pneumoniae (CRKP) poses one of the major challenges in clinical anti-infective therapy worldwide. This retrospective cohort study at a tertiary general hospital in Wuhan aimed to identify risk factors for hospital-acquired CRKP infections among 1,113 patients. All participants were aged 18 years and above, and had confirmed positive cultures for KP isolated within 48 hours post-hospitalization. Independent risk factors were identified using LASSO logistic regression and incorporated into a predictive nomogram. The factors included in the nomogram were prior carbapenem exposure, prior β-lactams-β-lactamase inhibitor combination (BLBLI) exposure, prior intensive care unit (ICU) stay, and prior mechanical ventilation. The areas under the receiver operating characteristic curve (AUC) for the nomogram were 0.793 in the training group (70% of patients) and 0.788 in the validation group (30% of patients), demonstrating its discriminatory power and predictive accuracy. The P values for the Hosmer-Lemeshow test were 0.333 and 0.684, indicating good calibration. The clinical utility of the nomogram was further supported by decision curve analysis (DCA) and clinical impact curve (CIC), demonstrating its potential to guide clinical decision-making. Our retrospective analysis identified key risk factors for CRKP infection and developed a nomogram that could effectively predict CRKP infections in hospitalized patients. Although the single-center nature of this study limits generalizability, the nomogram provides a foundation for future prospective, multicenter validations.IMPORTANCEWe established a nomogram scoring system that incorporates four key risk factors: prior carbapenem exposure, prior β-lactams-β-lactamase inhibitor combination (BLBLI) exposure, prior intensive care unit (ICU) stay, and prior mechanical ventilation. This nomogram demonstrated strong discriminatory power, excellent calibration, and significant clinical utility. This study highlights the critical risk factors associated with hospital-acquired carbapenem-resistant Klebsiella pneumoniae (CRKP) infections, providing valuable insights for clinicians to identify high-risk patients.
Keywords: Klebsiella pneumoniae; carbapenem resistance; nomogram; risk factor.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Lou T, Du X, Zhang P, Shi Q, Han X, Lan P, Yan R, Hu H, Wang Y, Wu X, Jiang Y, Yu Y. 2022. Risk factors for infection and mortality caused by carbapenem-resistant Klebsiella pneumoniae: a large multicentre case-control and cohort study. J Infect 84:637–647. doi: 10.1016/j.jinf.2022.03.010 - DOI - PubMed
-
- Lee C-R, Lee JH, Park KS, Jeon JH, Kim YB, Cha C-J, Jeong BC, Lee SH. 2017. Antimicrobial resistance of hypervirulent Klebsiella pneumoniae: epidemiology, hypervirulence-associated determinants, and resistance mechanisms. Front Cell Infect Microbiol 7:483. doi: 10.3389/fcimb.2017.00483 - DOI - PMC - PubMed
-
- Boix-Palop L, Xercavins M, Badía C, Obradors M, Riera M, Freixas N, Pérez J, Rodríguez-Carballeira M, Garau J, Calbo E. 2017. Emerging extended-spectrum β-lactamase-producing Klebsiella pneumoniae causing community-onset urinary tract infections: a case-control-control study. Int J Antimicrob Agents 50:197–202. doi: 10.1016/j.ijantimicag.2017.03.009 - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

