Antimicrobial Effects of Thonningianin a (TA)-Loaded Chitosan Nanoparticles Encapsulated by a PF-127 hydrogel in Diabetic Wound Healing
- PMID: 39651354
- PMCID: PMC11624675
- DOI: 10.2147/IJN.S488115
Antimicrobial Effects of Thonningianin a (TA)-Loaded Chitosan Nanoparticles Encapsulated by a PF-127 hydrogel in Diabetic Wound Healing
Abstract
Background and purpose: Diabetic wounds are serious chronic complications of diabetes and can lead to amputation and death. Although considerable progress has been made in drugs and materials for treating it, it's still an urgent clinical problem as the materials and drugs have potential therapeutic drawbacks, such as low delivery efficiency and poor tissue permeability. To promote diabetic wound healing, a composite of thonningianin A (TA)-loaded chitosan nanoparticles (CNPS) encapsulated by a Pluronic F-127 (PF-127) hydrogel (TA-CNPS-PF) was developed in this study.
Methods: TA-CNPS was prepared by ionic gelation method and TA-CNPS was thoroughly dispersed into PF-127 hydrogel to prepare TA-CNPS-PF. The particle size, hydrogel structure, encapsulation ratio, release ratio, antimicrobial properties of TA-CNPS-PF were determined and the effect of TA-CNPS-PF on diabetic wounds was assessed. The effect of TA on macrophage polarization was also examined in vitro.
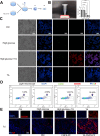
Results: The particle size was approximately 100 nm of TA-CNPS-PF and the hydrogel had a homogeneous three-dimensional reticulation structure. The encapsulation efficiency of TA in the CNPS were 99.3% and the release ratio of TA-CNPS-PF was approximately 86% and has antimicrobial properties. TA-CNPS-PF promoted diabetic wound healing significantly. Histopathology confirmed that TA-CNPS-PF promoted complete re-epithelialization and adequate collagen deposition. TA promoted the polarization of M1 macrophages into M2 macrophages via light microscopy, immunocytometry and flow cytometry. TA-CNPS-PF also promoted an increase in the number of M2 macrophages in diabetic wounds.
Conclusion: TA promotes diabetic wound healing by promoting the polarization of M1 macrophages into M2 macrophages and TA-CNPS-PF has good antimicrobial activity and a good drug release ratio in this study, which provides a new direction for the treatment of diabetic wounds and is expected to be highly advantageous in clinical diabetes wound therapy.
Keywords: M1 macrophages; M2 macrophages; TA nanoparticle hydrogel; TA-CNPS-PF; diabetic wound; thonningianin A. TA.
© 2024 Lin et al.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures




References
-
- Pawar KB, Desai S, Bhonde RR, Bhole RP, Deshmukh AA. Wound with diabetes: present scenario and future. Curr Diabetes Rev. 2021;17(2):136–142. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

