Association of chronic pain with incidence and progression of cardiometabolic multimorbidity in middle-aged and older populations: a multicohort study
- PMID: 39664712
- PMCID: PMC11630955
- DOI: 10.1097/PR9.0000000000001211
Association of chronic pain with incidence and progression of cardiometabolic multimorbidity in middle-aged and older populations: a multicohort study
Abstract
Introduction: Chronic pain is associated with single cardiometabolic diseases (CMDs). Less is known about the association of chronic pain with the co-occurrence of multiple CMDs, known as cardiometabolic multimorbidity (CMM).
Objectives: This study aims to examine the association between chronic pain and incidence of CMM and if it existed, to what extent chronic pain relates to the progression of specific CMD-related multimorbidity (MM).
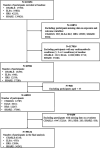
Methods: We pooled individual-level data of 59,134 participants from 4 cohort studies across 18 countries between 2010 and 2020. Participants aged 45 years or older, free of CMDs (diabetes, heart diseases, and stroke), and with self-reported chronic pain status at baseline were included. Multinomial logistic regression was performed on the association of chronic pain with incident CMM and the progression of specific CMD-related MM.
Results: One-third (21,204) of participants reported chronic pain at baseline. After 8 to 9 years, 1344 (2.3%) developed CMM. Chronic pain was associated with the onset of each CMD (odds ratio [OR] range 1.12-1.37) and CMM combinations (OR range 1.57-2.09). It is also linked with the increased odds of more CMDs (1, 2, and 3) during the follow-up. For example, OR increased from 1.31 for individuals with one CMD, to 1.57 for those with 2 CMDs, to 2.09 for those with 3 CMDs. Chronic pain was also associated with developing all CMD-related MM (OR range 1.26-1.88). Compared with those with diabetes only, participants with chronic pain were more likely to progress to diabetes and heart diseases, as well as diabetes, heart diseases, and stroke.
Conclusion: Chronic pain is associated with incidence and progression of CMM, whose management should be considered in primary and secondary prevention of CMM among middle-aged and older populations.
Keywords: Cardiometabolic multimorbidity; Chronic pain; Middle-aged and older adults; Multicohort.
Copyright © 2024 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of The International Association for the Study of Pain.
Conflict of interest statement
The authors have no conflict of interest to declare.Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
Figures



Similar articles
-
Chronic low-grade inflammation associated with higher risk and earlier onset of cardiometabolic multimorbidity in middle-aged and older adults: a population-based cohort study.Sci Rep. 2024 Sep 30;14(1):22635. doi: 10.1038/s41598-024-72988-7. Sci Rep. 2024. PMID: 39349699 Free PMC article.
-
Role of sarcopenia in Temporal progression trajectory of cardiometabolic diseases: a prospective study in UK biobank.BMC Public Health. 2025 Apr 7;25(1):1294. doi: 10.1186/s12889-025-22500-1. BMC Public Health. 2025. PMID: 40189542 Free PMC article.
-
Duration-dependent impact of cardiometabolic diseases and multimorbidity on all-cause and cause-specific mortality: a prospective cohort study of 0.5 million participants.Cardiovasc Diabetol. 2023 Jun 12;22(1):135. doi: 10.1186/s12933-023-01858-9. Cardiovasc Diabetol. 2023. PMID: 37308998 Free PMC article.
-
Frailty, an Independent Risk Factor in Progression Trajectory of Cardiometabolic Multimorbidity: A Prospective Study of UK Biobank.J Gerontol A Biol Sci Med Sci. 2023 Oct 28;78(11):2127-2135. doi: 10.1093/gerona/glad125. J Gerontol A Biol Sci Med Sci. 2023. PMID: 37170845
-
Serum/plasma biomarkers and the progression of cardiometabolic multimorbidity: a systematic review and meta-analysis.Front Public Health. 2023 Nov 23;11:1280185. doi: 10.3389/fpubh.2023.1280185. eCollection 2023. Front Public Health. 2023. PMID: 38074721 Free PMC article.
Cited by
-
Exploring the association between dietary caffeine and chronic musculoskeletal pain: a cross-sectional analysis of NHANES.Front Nutr. 2025 Apr 28;12:1570403. doi: 10.3389/fnut.2025.1570403. eCollection 2025. Front Nutr. 2025. PMID: 40357035 Free PMC article.
-
Social Connection and Chronic Pain: A Cohort Study to Explore the Association of Social Isolation and Loneliness with Chronic Pain Among Older Adults in China.J Pain Res. 2025 Aug 20;18:4187-4199. doi: 10.2147/JPR.S526555. eCollection 2025. J Pain Res. 2025. PMID: 40860503 Free PMC article.
References
-
- Bouhassira D, Lantéri-Minet M, Attal N, Laurent B, Touboul C. Prevalence of chronic pain with neuropathic characteristics in the general population. PAIN 2008;136:380–7. - PubMed
-
- Busija L, Lim K, Szoeke C, Sanders KM, McCabe MP. Do replicable profiles of multimorbidity exist? Systematic review and synthesis. Eur J Epidemiol 2019;34:1025–53. - PubMed
-
- Cohen SP, Vase L, Hooten WM. Chronic pain: an update on burden, best practices, and new advances. Lancet (London, England) 2021;397:2082–97. - PubMed
LinkOut - more resources
Full Text Sources
