Epidemiological profile of kidney transplant patients with lupus nephritis
- PMID: 39671453
- PMCID: PMC11642653
- DOI: 10.1590/2175-8239-JBN-2024-0061en
Epidemiological profile of kidney transplant patients with lupus nephritis
Abstract
Introduction: Lupus nephritis (LN) affects up to 50% of patients with systemic lupus erythematosus (SLE) and may lead to kidney failure and require kidney transplantation (KT). Results compared to KT from other causes are controversial, and we aimed to assess the clinical course, complications, and survival of LN patients undergoing KT.
Methodology: Retrospective cohort of 99 KT due to LN from 1977 to 2023 at a single center, divided into two groups according to the immunosuppression period: G1 (before 2009) and G2 (from 2009 onwards). Clinical and demographic characteristics, as well as clinical evolution, were compared.
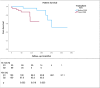
Results: Patients were predominantly white (65.9%), female (86.9%), in their first KT (83.8%). The median age was 20.0 (11.5-25.0) years at SLE diagnosis, and 30.0 (23.0-40.0) years at KT. Renal graft biopsy was indicated in 46% of patients, with rejection observed in 23%, and LN recurrence in 5%. When assessing the two distinct periods of standard immunosuppression, there was no difference in median glomerular filtration rate and proteinuria at 1 and 5 years, nor in 5-year survival. Throughout follow-up, 37.4% of patients lost their graft, and 13% died with a functioning graft. No graft loss was attributed to LN recurrence.
Conclusion: KT is a successful treatment for LN, with graft survival rates similar to those of transplants from other causes. LN recurrence was not associated with renal graft loss.
Introdução: A nefrite lúpica (NL) afeta até 50% dos pacientes com lúpus eritematoso sistêmico (LES) e pode levar à falência renal e necessidade de transplante renal (TR). Os resultados em comparação à TR por outras causas são controversos, e visamos avaliar evolução clínica, complicações e sobrevida de pacientes com NL submetidos a TR.
Metodologia: Coorte retrospectiva de 99 TR por NL de 1977 a 2023 em um único centro, divididos em dois grupos conforme o período de imunossupressão: G1 (antes de 2009) e G2 (a partir de 2009). As características clínicas, demográficas e evolução clínica foram comparadas.
Resultados: Pacientes eram na maioria brancos (65,9%), sexo feminino (86,9%), no primeiro TR (83,8%). A idade mediana foi 20,0 (11,5–25,0) anos no diagnóstico de LES e 30,0 (23,0–40,0) anos no TR. Biópsia do enxerto renal foi indicada para 46% dos pacientes, com rejeição em 23% e recorrência de NL em 5%. Avaliando os dois períodos distintos de imunossupressão padrão, não houve diferença na mediana de taxa de filtração glomerular e de proteinúria em 1 ano e em 5 anos, nem da sobrevida em 5 anos. Em todo o acompanhamento, 37,4% dos pacientes perderam o enxerto e 13% morreram com enxerto funcionante. Nenhuma perda foi atribuída à recorrência de NL.
Conclusão: TR é um tratamento bem-sucedido na NL, com taxas de sobrevida do enxerto semelhantes às de transplantes por outras causas. A recorrência de NL não esteve associada à perda do enxerto renal.
Conflict of interest statement
The authors declare no conflict of interest.
Figures



References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

