Dural Venous Sinus Thrombosis: A Rare Cause of Intracranial Hemorrhage
- PMID: 39677148
- PMCID: PMC11646077
- DOI: 10.7759/cureus.73693
Dural Venous Sinus Thrombosis: A Rare Cause of Intracranial Hemorrhage
Abstract
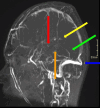
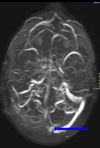
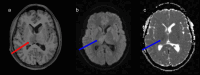
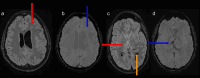
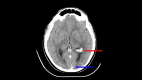
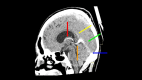
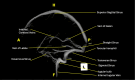
Dural venous sinus thrombosis, a subset of cerebral venous thrombosis, is an important pathology due to its significant morbidity and mortality. This process has an annual incidence of three to five cases per million adults. Although copious predisposing factors exist, the core principles revolve around Virchow's triad: venous stasis, hypercoagulability, and vascular endothelial damage. There are various risk factors related to unfavorable outcomes, which include female sex, intracranial hemorrhage, infection, cancer, and more. Trauma tends to be a risk factor, particularly in pediatric populations, as in this patient's case. Initial diagnosis in the acute setting commonly involves non-contrast CT studies to exclude hemorrhage. In subacute or chronic settings, MRI can be utilized. Anticoagulation remains the mainstay of therapy for treatment, along with treating any underlying causes of thrombosis. We present a pediatric patient with extensive post-traumatic dural venous sinus thromboses with classic imaging findings as well as full resolution of clinical symptoms after this pathologic process was recognized and treated appropriately.
Keywords: dural vein; head trauma; mr venography; pediatric head injury; sinus thrombosis.
Copyright © 2024, Alam et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
Similar articles
-
Cerebral venous congestion as indication for thrombolytic treatment.Cardiovasc Intervent Radiol. 2007 Jul-Aug;30(4):675-87. doi: 10.1007/s00270-007-9046-1. Cardiovasc Intervent Radiol. 2007. PMID: 17573553
-
Pediatric cerebral venous sinus thrombosis or compression in the setting of skull fractures from blunt head trauma.J Neurosurg Pediatr. 2018 Mar;21(3):258-269. doi: 10.3171/2017.9.PEDS17311. Epub 2017 Dec 15. J Neurosurg Pediatr. 2018. PMID: 29243974
-
Traumatic cerebral dural sinus vein thrombosis/stenosis in pediatric patients-is anticoagulation necessary?Childs Nerv Syst. 2021 Sep;37(9):2847-2855. doi: 10.1007/s00381-021-05204-w. Epub 2021 May 14. Childs Nerv Syst. 2021. PMID: 33990877
-
Nontraumatic vascular emergencies: imaging and intervention in acute venous occlusion.Eur Radiol. 2002 Nov;12(11):2627-43. doi: 10.1007/s00330-002-1615-8. Epub 2002 Aug 22. Eur Radiol. 2002. PMID: 12386751 Review.
-
Cerebrovascular complications in cancer patients.Neurol Clin. 2003 Feb;21(1):167-92. doi: 10.1016/s0733-8619(02)00066-x. Neurol Clin. 2003. PMID: 12690649 Review.
References
-
- Craniocervical vascular anatomy. San Millán Ruiz D, Barnett BP, Gailloud P. Image-Guided Interventions: Expert Radiology Series, Third Edition. 2020:454–472.
-
- Cerebral venous thrombosis: a comprehensive review. Idiculla PS, Gurala D, Palanisamy M, Vijayakumar R, Dhandapani S, Nagarajan E. Eur Neurol. 2020;83:369–379. - PubMed
-
- Cerebral venous sinus thrombosis risk factors. Saadatnia M, Fatehi F, Basiri K, Mousavi SA, Mehr GK. Int J Stroke. 2009;4:111–123. - PubMed
-
- Cerebral venous sinus thrombosis in closed head injury: systematic review and meta-analysis. Alghamdi SR, Cho A, Lam J, Al-Saadi T. J Clin Neurosci. 2022;98:254–260. - PubMed
-
- Cerebral venous sinus thrombosis. Capecchi M, Abbattista M, Martinelli I. J Thromb Haemost. 2018;16:1918–1931. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
