2'-Hydroxycinnamaldehyde, a Natural Product from Cinnamon, Alleviates Ischemia/Reperfusion-Induced Microvascular Dysfunction and Oxidative Damage in Rats by Upregulating Cytosolic BAG3 and Nrf2/HO-1
- PMID: 39684673
- PMCID: PMC11641319
- DOI: 10.3390/ijms252312962
2'-Hydroxycinnamaldehyde, a Natural Product from Cinnamon, Alleviates Ischemia/Reperfusion-Induced Microvascular Dysfunction and Oxidative Damage in Rats by Upregulating Cytosolic BAG3 and Nrf2/HO-1
Abstract
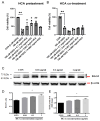
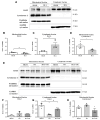
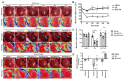
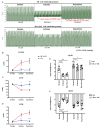
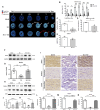
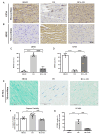
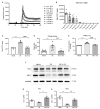
2'-Hydroxycinnamaldehyde (HCA), a natural product isolated from the bark of Cinnamomum cassia, has anti-inflammatory and anti-tumor activities. In this study, we explored whether HCA preconditioning could protect the heart against ischemia/reperfusion (I/R)-induced oxidative injury through cytosolic Bcl-2-associated athanogene 3 (BAG3) upregulation. In vivo HCA preconditioning was performed intraperitoneally in adult male Wistar rats (50 mg/kg body weight) three times/week for 2 weeks before cardiac I/R injury. The animals were divided into sham control (sham), I/R, and HCA preconditioning plus I/R (HCA+I/R) groups. We examined left ventricular pressure cardiac hemodynamics, the microcirculation, electrocardiograms, infarct size, and oxidative stress and performed Western blots, immunohistochemistry, and cytokine array assays. HCA pretreatment, via BAG3 overexpression, inhibited H2O2-induced H9c2 cell death. Cardiac I/R injury increased ST-segment elevation, left ventricular end-diastolic pressure, infarct size, myocardial disruption, tissue edema, erythrocyte accumulation, leukocyte infiltration, reactive oxygen species, malondialdehyde, 8-isoprostane, caspase 3-mediated apoptosis, 4HNE/GPX4-mediated ferroptosis, and fibrosis but decreased the microcirculation, cytosolic BAG3, and Beclin-1/LC3 II-mediated autophagy in the I/R hearts. HCA preconditioning significantly decreased these oxidative injuries by increasing cardiac cytosolic BAG3 and Nrf2/HO-1 signaling. HCA preconditioning significantly decreased cardiac I/R-enhanced mitochondrial fission DRP1 expression. Our data suggest that HCA preconditioning can efficiently improve myocardial I/R injury-induced cardiac dysfunction, apoptosis, ferroptosis, mitochondrial fission, and autophagy inhibition through cardiac BAG3 and Nrf2/HO-1 upregulation.
Keywords: 2′-Hydroxycinnamaldehyde; Bcl-2-associated athanogene 3; apoptosis; autophagy; ferroptosis; myocardial ischemia/reperfusion injury; natural product.
Conflict of interest statement
All the authors declare no potential conflicts of interest.
Figures



References
-
- Luan F., Lei Z., Peng X., Chen L., Peng L., Liu Y., Rao Z., Yang R., Zeng N. Cardioprotective effect of cinnamaldehyde pretreatment on ischemia/reperfusion injury via inhibiting NLRP3 inflammasome activation and gasdermin D mediated cardiomyocyte pyroptosis. Chem. Interact. 2022;368:110245. doi: 10.1016/j.cbi.2022.110245. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

