Efficacy and safety of oral propranolol and topical timolol in the treatment of infantile hemangioma: a meta-analysis and systematic review
- PMID: 39687294
- PMCID: PMC11646719
- DOI: 10.3389/fphar.2024.1515901
Efficacy and safety of oral propranolol and topical timolol in the treatment of infantile hemangioma: a meta-analysis and systematic review
Abstract
Background: Propranolol, a nonselective β-blocker, is the first-line treatment for infantile hemangioma (IH). Topical timolol has recently been proposed as a novel IH treatment with fewer adverse effects. This study was conducted to compare the efficacy and safety of oral propranolol and topical timolol for treating IH.
Methods: Studies were included after searching PubMed, Embase, Web of Science, and the Cochrane Library via the keywords of "propranolol", "timolol", "infantile hemangioma" and their synonyms. A meta-analysis with pooled odds ratios was performed using the fixed-effect model.
Results: Seven articles with 2071 patients were included in this meta-analysis. Compared with topical timolol, oral propranolol had a greater response rate (OR = 2.12, P < 0.001), but it was also associated with a greater risk of adverse events (OR = 2.31, P < 0.001). For superficial IH, timolol demonstrated similar efficacy to propranolol (OR = 1.28, P = 0.34) but with fewer adverse events (OR = 2.30, P = 0.001). Additionally, compared with topical timolol, propranolol at a dosage of 2 mg/kg/d had a better response rate (OR = 2.62, P < 0.001), whereas the 1.0∼1.5 mg/kg/d propranolol group showed no significant difference (OR = 1.34, P = 0.38).
Conclusion: Oral propranolol presents superior therapeutic efficacy in the treatment of IH compared to topical timolol. However, topical timolol can serve as an alternative to oral propranolol for treating superficial IH, providing similar efficacy with fewer adverse effects. Additionally, propranolol at a dosage of 2 mg/kg/d offers greater efficacy with a comparable safety profile, whereas the 1.0∼1.5 mg/kg/d propranolol dosage shows no significant difference in efficacy compared to timolol but is associated with more adverse events.
Systematic review registration: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42024603724, identifier CRD42024603724.
Keywords: efficacy and safety; infantile hemangioma; meta-analysis; propranolol; timolol.
Copyright © 2024 Huang, Si, Zou, Li, Mu, Zhong and Yang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
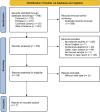




References
Publication types
LinkOut - more resources
Full Text Sources

