Acute Sarcopenia: Systematic Review and Meta-Analysis on Its Incidence and Muscle Parameter Shifts During Hospitalisation
- PMID: 39690131
- PMCID: PMC11695106
- DOI: 10.1002/jcsm.13662
Acute Sarcopenia: Systematic Review and Meta-Analysis on Its Incidence and Muscle Parameter Shifts During Hospitalisation
Abstract
Background: Acute sarcopenia is sarcopenia lasting less than 6 months, typically following acute illness or injury. It may impact patient recovery and quality of life, advancing to chronic sarcopenia. However, its development and assessment remain poorly understood, particularly during hospitalisation. This systematic review aimed to elucidate the incidence of acute sarcopenia and examine changes in muscle parameters during hospitalisation.
Methods: Eighty-eight papers were included in the narrative synthesis; 33 provided data for meta-analyses on the effects of hospitalisation on handgrip strength (HGS), rectus femoris cross-sectional area (RFCSA) and various muscle function tests. Meta-regressions were performed for length of hospital stay (LoS) and age for all meta-analyses; sex was also considered for HGS.
Results: Acute sarcopenia development was assessed in four studies with a pooled incidence of 18% during hospitalisation. Incidence was highest among trauma patients in intensive care (59%), whereas it was lower among medical and surgical patients (15%-20%). Time of development ranged from 4 to 44 days. HGS remained stable during hospitalisation (SMD = 0.05, 95% CI = -0.18:0.28, p = 0.67) as did knee extensor strength. LoS affected HGS performance (θ = 0.04, 95% CI = 0.001:0.09, p = 0.045) but age (p = 0.903) and sex (p = 0.434) did not. RFCSA, reduced by 16.5% over 3-21 days (SMD = -0.67, 95% CI = -0.92:-0.43, p < 0.001); LoS or time between scans did significantly predict the reduction (θ = -0.04, 95% CI = -0.077:-0.011, p = 0.012). Indices of muscle quality also reduced. Muscle function improved when assessed by the short physical performance battery (SMD = 0.86, 95% CI = 0.03:1.69, p = 0.046); there was no change in 6-min walk (p = 0.22), timed up-and-go (p = 0.46) or gait speed tests (p = 0.98). The only significant predictor of timed up-and-go performance was age (θ = -0.11, 95% CI = -0.018:-0.005, p = 0.009).
Conclusions: Assessment and understanding of acute sarcopenia in clinical settings are limited. Incidence varies between clinical conditions, and muscle parameters are affected differently. HGS and muscle function tests may not be sensitive enough to identify acute changes during hospitalisation. Currently, muscle health deterioration may be underdiagnosed impacting recovery, quality of life and overall health following hospitalisation. Further evaluation is necessary to determine the suitability of existing diagnostic criteria of acute sarcopenia. Muscle mass and quality indices might need to become the primary determinants for muscle health assessment in hospitalised populations.
Keywords: atrophy; cachexia; disuse; wasting; weakness.
© 2025 The Author(s). Journal of Cachexia, Sarcopenia and Muscle published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

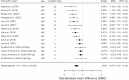
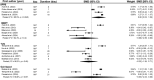
References
-
- Lee Z. Y., Ong S. P., Ng C. C., et al., “Association Between Ultrasound Quadriceps Muscle Status With Premorbid Functional Status and 60‐Day Mortality in Mechanically Ventilated Critically Ill Patient: A Single‐Center Prospective Observational Study,” Clinical Nutrition 40 (2021): 1338–1347. - PubMed
-
- Srikanthan P., Horwich T. B., and Tseng C. H., “Relation of Muscle Mass and Fat Mass to Cardiovascular Disease Mortality,” American Journal of Cardiology 117 (2016): 1355–1360. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

